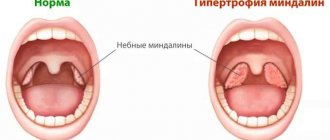
Bends, as well as bends of such a structure as the gallbladder, are characterized by a violation of the anatomical structure of the organ with a general decrease in its functional state. The structure of the gallbladder is divided into three components: the neck, the fundus and the body itself. When filled, the properly positioned gallbladder takes on a pear-shaped shape. The bending condition leads to its deformation and partial or complete change in the correct shape of the bubble. This phenomenon is characterized as an inflection or bend of this organ. A kink in the gallbladder is common in children.
What is inflection?
Bend of the gallbladder: ultrasound
Excesses in the gallbladder are both congenital and acquired as a result of a number of environmental factors. If it is congenital, the bend can be detected completely in a newborn baby and corrected. Such natural disorders are diagnosed by computer research using an ultrasound procedure. Since children's organs are formed by interacting with each other, a change in the shape of the gallbladder will not interfere with its normal functioning and will not cause any problems. The acquired nature of excesses in the gallbladder must be treated. Most often, treatment is lengthy and labor-intensive.
Twisting resulting from any reason prevents the patient from leading a full life, due to disruption of the outflow of the bile flow and disruption of the digestive tract.
Short frenulum of the tongue - how to determine?
Symptoms of a tongue frenulum are usually identified by a speech therapist during a myofunctional examination. Most often, specialists (this can be attentive parents or the patient himself) observe the following symptoms:
- Limitation of tongue mobility; it is difficult for the patient to move the tongue out of the mouth and raise the tip of the tongue to the upper lip.
- The tip of the tongue bifurcates when you try to push it forward.
- The patient pronounces the sound L incorrectly, making it sound like V.
- Sometimes a short frenulum of the tongue brings purely everyday discomfort, as in the clinical case described above.
Why do kinks occur?
As mentioned earlier, this pathology can be congenital or acquired. Birth defects occur under the influence of a person’s genotype and negative factors during intrauterine development. Typically, congenital abnormalities do not cause additional discomfort to a person, and may disappear on their own in childhood. Acquired kinks in the bladder in children can occur for the following reasons:
- prolonged emotional stress in a child;
- excessive physical activity;
- severe obesity;
- violation of proper diet;
- backbreaking physical labor;
- exacerbation of chronic cholecystitis.
In childhood, there is no need to lift excessive weight, as this can provoke prolapse of internal organs and affect the appearance of kinks in the gallbladder. Acquired kinks cause discomfort and must be treated.
Gallstone disease that develops in childhood can also lead to twisting of the bladder. In this case, the gallbladder begins to sag under the influence of gravity of the formed stones and, as a result, an inevitable bend of the cervical part of the organ occurs. In case of this pathology, you should immediately seek advice from a medical institution, otherwise a violation of the outflow of bile formed in the body in most cases leads to problems in the functioning of all digestive organs.
Signs of kinks
Compliance with a diet for gallstone inflection is the main condition for treatment
If there are kinks in the gallbladder, the child feels pain at the site of the twisting of the organ. Pain appears in the right side, back and shoulder blades. If, during the bend, bile enters the peritoneum, then severe abdominal pain is felt, moving to the left region. Over time, the pain may subside and then reappear. The child experiences bloating in the abdominal cavity, pain, as well as sudden changes in body temperature and abnormal bowel movements. These symptoms indicate a bend in the cervical region of the bladder.
If the deformation of the gallbladder is caused by the onset of an inflammatory process, then changes in skin color occur, causing it to acquire an earthy tint. Symptoms of pain are associated with the location of the bend. Let's consider the main areas where defects occur, as well as their symptomatic signs:
- If the bend occurs in the border area of the body and the bottom of the gallbladder, then the sick child feels pain in the abdominal region, in the collarbone, sternum and under the scapula. Attacks of nausea and vomiting are frequent, usually occurring after meals. A kind of plaque forms on the outer surface of the child’s tongue, and cracks also appear in the outer corners of the oral cavity. This type of pathology most often occurs in childhood.
- If twisting of the gallbladder occurs in its cervical region, then the most common manifestations of pain in the left hypochondrium, accompanied by nausea and increased gas formation, become apparent.
- There are times when the patient even develops a feverish state. A bend in the neck is the most dangerous and life-threatening, since it is possible for the resulting bile to penetrate into the abdominal cavity, accompanied by the formation of peritonitis in the body.
- If a combined type of inflection is observed, which represents numerous deformations of the gallbladder in its different areas, then the patient experiences severe abdominal pain. Sometimes meals are accompanied by nausea and a gag reflex.
STRIDOR in newborns and children of the first year of life
Stridor is a rough, variable-pitched sound caused by turbulent air flow as it passes through a narrowed area of the airway [36]. Stridor in newborns and infants is a pathology that is a symptom of respiratory obstruction [7]. Stridor can be a symptom of life-threatening illnesses. The most important characteristics of stridor are its volume, pitch, and the breathing phase at which it occurs.
Loud stridor is usually a symptom of severe airway narrowing. In the case of progressively worsening stridor, a sudden weakening of the sound may be a sign of increased obstruction, weakening of respiratory movements and the occurrence of airway collapse [28].
High-sounding stridor is usually caused by obstruction at the level of the vocal folds [26], while low-sounding stridor is usually caused by pathology above the vocal folds (the laryngeal part of the pharynx, the upper part of the larynx). Mid-range stridor is most often a symptom of obstruction below the vocal folds [41].
The most important sign to suspect the level of damage is the respiratory phase in which stridor is best heard. On this basis, stridor can be divided into three types: inspiratory, expiratory and biphasic. Inspiratory stridor is usually caused by a lesion located above the vocal folds and is produced by the collapse of soft tissue under negative pressure during inspiration [22]. Biphasic stridor is usually high-pitched. It is caused by a lesion at the level of the vocal folds or subglottic region [16, 18]. Expiratory stridor occurs more often with damage to the lower respiratory tract [42].
History is very important for diagnosing the disease. Key historical data are the reasons and duration of intubation (if previously performed) in the neonatal period. Other anamnestic features include age at onset of stridor, duration of stridor, association with crying or feeding, and position of the child; the presence of other associated symptoms, such as coughing paroxysms, aspiration or regurgitation [40, 41].
When examining a child, you should evaluate his general condition, respiratory and heart rate, and skin color. In addition, you should pay attention to possible anomalies in the structure of the head, the participation of additional muscles in the act of breathing, retraction of the compliant areas of the chest and other signs, and exclude a possible infectious disease [36].
If the child’s condition does not require immediate intervention, an x-ray of the larynx and soft tissues of the neck in the anterior and lateral projection, chest, as well as x-ray of the esophagus with a water-soluble radiopaque substance should be performed. In addition, ultrasound examination of the larynx, computed tomography, and nuclear magnetic resonance may be useful [12, 30].
The most informative method for diagnosing a disease manifested by congenital stridor is endoscopic examination: fiberoscopy; direct laryngoscopy under anesthesia, preferably using a microscope; tracheobroncho- and esophagoscopy [11, 36]. In this case, it is necessary to take into account the possibility of an abnormal structure of several parts of the respiratory tract [23, 25].
- The most common causes of stridor in newborns and infants
| Figure 1. Endophotograph of the larynx. Soft epiglottis extending into the airway |
Laryngomalacia is the most common cause of stridor [16, 30]. Anatomically, the following forms of laryngomalacia can be distinguished: due to the retraction of the soft epiglottis into the lumen of the larynx (Fig. 1); due to the arytenoid cartilages, when inhaling, they are pulled up or pulled up initially, due to the shortened aryepiglottic fold (Fig. 2); mixed form, when both the epiglottis and arytenoid cartilages fall into the lumen of the respiratory tract. Laryngomalacia usually occurs
| Figure 2. Endophotograph of the larynx. Arytenoid cartilages extending into the lumen of the larynx |
“benign” and disappears spontaneously, usually by 1.5 - 2 years of life.
Boys are affected twice as often as girls. Stridor usually appears from birth, but in some cases it does not occur until the second month of life. Symptoms may be transient and worsen when the child lies on his back or during crying and agitation. The severity of the disease may vary. Most children experience only noisy, sonorous breathing, but in some cases laryngomalacia causes laryngeal stenosis, requiring intubation and even tracheotomy. In severe cases, surgical treatment is resorted to, usually using a laser - making incisions on the epiglottis, dissecting the aryepiglottic folds or removing part of the arytenoid cartilages. Vocal fold paralysis is the second most common cause of congenital stridor [39, 41]. It is usually found in children with other congenital anomalies or central nervous system involvement [29]. Often the cause of paralysis remains unclear, and this type of paralysis is considered idiopathic. In cases of idiopathic paralysis (possibly caused by birth trauma), it is often
| Figure 3. Endophotograph of the larynx. Right arytenoid fold paralysis |
spontaneous healing occurs.
In other cases, the cause may be hemorrhages in the ventricles of the brain, meningoencephalocele, hydrocephalus, perinatal encephalopathy and other diseases [29]. In addition, iatrogenicity (for example, when the recurrent laryngeal nerve is damaged) can be identified as the cause of the development of vocal fold paralysis. Bilateral paralysis causes high-pitched stridor and aphonia. About half of children with bilateral paralysis require tracheotomy [22, 26, 39].
With unilateral paralysis (Fig. 3), a weak cry is usually noted, the voice gradually improves with age. Respiratory function is usually not affected by unilateral paralysis [28].
| Figure 4. Endophotograph of the larynx. Congenital scar membrane of the larynx |
Congenital cicatricial membrane (Fig. 4) and subglottic stenosis develop as a result of incomplete separation of the germinal mesenchyme between the two walls of the developing larynx [33]. Acquired cicatricial stenoses are found much more often (Fig. 5), usually developing as a result of prolonged transglottic nasotracheal intubation. The severity of the disease depends on the degree of damage: a small scar membrane, localized only in the area of the anterior commissure, is clinically manifested only by a change in voice (“cock crow”); complete laryngeal atresia is compatible with life only theoretically [30].
| Figure 5. Endophotograph of the larynx. Acquired subglottic stenosis (pinpoint airway lumen) |
The leading clinical symptoms of the disease are obstruction of the upper respiratory tract, such as biphasic stridor, tachypnea, cyanosis, anxiety, flaring of the wings of the nose when breathing, participation of auxiliary muscles in the act of breathing, etc. When the membrane is localized in the area of the vocal folds, voice disorders up to aphonia are noted .
The leading diagnostic method is endoscopy [30], although radiography of the larynx and trachea in anterior and lateral projections indirectly helps.
| Figure 6. Endophotograph of the larynx. Cyst of the lingual surface of the epiglottis |
Treatment is determined by the severity of symptoms. Only children with small anterior commissural synechiae can be kept under observation without surgical treatment; patients with a medium-sized membrane that causes breathing problems require surgical treatment (usually laser destruction) during the neonatal period. Children with severe membrane usually require tracheotomy in the neonatal period followed by surgery (using a laser or external approach) at an older age [17, 38].
| Figure 7. Endophotograph of the larynx. Right vocal fold cyst |
In some cases, congenital subglottic stenosis is accompanied by other congenital lesions [34]. When choosing treatment tactics, it is necessary to take into account that breathing can improve with the growth of the larynx.
Laryngeal cysts. Stridor occurs when a cyst grows into the lumen of the respiratory tract or compression of the soft tissues of the larynx. In addition, when localized on the laryngeal and especially on the lingual surface of the epiglottis (Fig. 6), they can cause dysphagic phenomena [20, 30].
The localization of cysts can be varied - epiglottis, supraglottic region, aryepiglottic folds, subglottic region. Often cysts develop in children with a history of intubation, and in such cases they can be multiple. Small cysts of the vocal folds (Fig. 7) are clinically manifested only by hoarseness. With mirror laryngoscopy, especially if the submucosal cyst is localized at the border of the anterior and middle third of the vocal fold, it is mistakenly diagnosed as a “singing” nodule. In this case, the correct diagnosis can only be established by examining the larynx under anesthesia using optics.
| Figure 8. Endophotograph of the larynx. Subglottic hemangioma under the left vocal fold |
For treatment, aspiration of the cyst contents is used, followed by excision of its walls with microinstruments or a CO2 laser [6, 8, 30].
Cysts often recur. In some cases, external surgery is required to excise large multiple recurrent cysts [31].
Subglottic hemangioma (Fig. threatens the life of the child. According to foreign literature, the average mortality from this disease is 8.5% [43]. In most cases, subglottic hemangioma is present from birth and undergoes growth during the first months of life. Stridor usually appears at 2 -3 months of life, the first symptoms of the disease are usually mistakenly diagnosed as croup [27]. In three of our cases, respiratory stenosis developed on the first day after cryodestruction of skin hemangiomas. Stridor is usually biphasic, the voice may not be changed. More than half of the children have skin hemangiomas. How and with skin hemangiomas, girls suffer three times more often than boys [9].The severity of the disease depends on the size of the hemangioma, in the case of acute respiratory viral infection or anxiety, breathing may worsen.
threatens the life of the child. According to foreign literature, the average mortality from this disease is 8.5% [43]. In most cases, subglottic hemangioma is present from birth and undergoes growth during the first months of life. Stridor usually appears at 2 -3 months of life, the first symptoms of the disease are usually mistakenly diagnosed as croup [27]. In three of our cases, respiratory stenosis developed on the first day after cryodestruction of skin hemangiomas. Stridor is usually biphasic, the voice may not be changed. More than half of the children have skin hemangiomas. How and with skin hemangiomas, girls suffer three times more often than boys [9].The severity of the disease depends on the size of the hemangioma, in the case of acute respiratory viral infection or anxiety, breathing may worsen.
The leading diagnostic method is endoscopy. Usually a pink or red soft tissue protrusion is found under the vocal fold (usually under the left) [5]. If the child has been previously intubated due to respiratory stenosis, the hemangioma may not be diagnosed when examining the airway immediately after extubation.
Treatment uses CO2 laser destruction of hemangioma followed by hormonal therapy [6, 24]. In case of hemangioma of the anterior surface of the neck that grows into the larynx, tracheotomy is necessary, followed by close-focus radiotherapy or treatment with corticosteroids [2].
| Figure 9. Endophotograph of the larynx. Juvenile respiratory papillomatosis |
Juvenile respiratory papillomatosis (JRP) (Fig. 9) is the most common tumor of the upper respiratory tract in children. The etiological factor of papillomatosis is the human papillomavirus, most often types 6 and 11 [3]. Although in the vast majority of patients the first symptoms of the disease develop at 2–3 years of life, in some cases we can talk about congenital laryngeal papillomatosis, when the first symptoms of the disease are noted from the moment of birth [1].
The initial symptom of the disease is usually hoarseness, gradually turning into aphonia. Subsequently, as papillomas grow and the lumen of the glottis narrows (obstructive form), progressive laryngeal stenosis occurs, manifesting itself as inspiratory or biphasic stridor [10].
The most common primary localization of laryngeal papillomas is the area of the commissure and the anterior third of the vocal folds. At later stages of the disease, papillomas can affect all parts of the larynx, as well as extend beyond its limits. Papillomas usually have a wide base, but the growth of conglomerates of papillomas on a small stalk is possible. In appearance, papillomas resemble a mulberry or a bunch of grapes. During microlaryngoscopy, the surface of papillomas is usually uneven, fine-grained or finely lobed, the color is often pale pink, sometimes with a grayish tint. The severity of the disease is determined by the growth rate of papillomas and the frequency of recurrence [15].
The main method of eliminating stenosis in children with JRP is surgical removal of papillomas using microinstruments and/or a CO2 laser. However, surgical treatment alone does not prevent relapse of the disease in most patients. Currently, the most pathogenetically justified and promising is long-term continuous administration of interferon drugs [13, 19, 21].
Tracheomalacia. There are diffuse and local forms of tracheomalacia, i.e. weakness of the tracheal wall associated with the pathological softness of its cartilaginous frame. Clinically, the disease manifests itself as expiratory stridor. During endoscopy, a sharp narrowing of the tracheal lumen is detected during exhalation, which can take various shapes. Symptoms of the disease often disappear spontaneously by 2–3 years of life [32]. Severe respiratory distress may require tracheotomy [41].
| Figure 10. Endophotograph of the trachea. Congenital cicatricial stenosis |
Congenital tracheal stenosis (Fig. 10) can have a different nature. Organic stenoses are associated with a local defect in the cartilaginous half-rings of the trachea (lack or absence of cartilage) or excessive formation of cartilage tissue, leading to the formation of a hard cartilaginous protrusion into the tracheal lumen [42].
Functional stenoses are associated with excessive softness of the cartilage and in this case are a local form of tracheomalacia. Expiratory stridor is usually detected immediately after birth. Stridor gets worse when the baby is restless or feeding. The patient's condition usually worsens sharply during ARVI; in some cases, attacks of suffocation are noted, which are mistakenly diagnosed as croup. To exclude external compression of the trachea, an X-ray contrast examination of the esophagus is necessary. The main diagnostic method is endoscopic. Tracheal stenosis, especially due to tracheomalacia, has a favorable prognosis and, in most cases, heals spontaneously.
| Figure 11. Chest X-ray. Compression of the esophagus by an abnormally located vessel |
Vascular ring. The abnormal configuration of large vessels can cause compression of the trachea, usually its distal parts.
In addition, the esophagus may also be compressed. Stridor gets worse when crying or feeding, or when the baby is lying on his back. Regurgitation is often noted. The diagnosis is established using radiography of the esophagus with a radiopaque agent (Fig. 11) and aortography. The most common type of aortic arch duplication is the accessory left pulmonary artery [14, 37]. During endoscopy, bulging and, in some cases, pulsation of the anterior wall of the trachea can be detected. Treatment is surgical.
Laryngotracheoesophageal hiatus is a rare congenital developmental defect. Over a long distance, the respiratory tract communicates with the esophagus. The cause of this defect is non-fusion of the dorsal part of the cricoid cartilage. This disease is clinically manifested by moderately loud biphasic stridor and episodes of aspiration. Children with this defect often experience repeated pneumonia. Paroxysms of cough and cyanosis are typical. The voice is quiet. Approximately 20% of children also have a tracheoesophageal fistula, typically located in the distal trachea [35]. To establish a diagnosis, in addition to endoscopy, chest X-ray with contrast is required. Treatment requires not only a tracheotomy, but also a gastrostomy tube to feed the child.
| Figure 12. Chest X-ray. Flow of radiopaque substance through the tracheoesophageal fistula from the esophagus into the tracheobronchial tree |
Tracheoesophageal fistula (Fig. 12) manifests itself during the first feeding of the child with severe attacks of suffocation, coughing and cyanosis [41]. The defect is based on incomplete development of the tracheoesophageal wall. Often this defect is combined with esophageal atresia. Subsequently, severe aspiration pneumonia quickly follows. Treatment is surgical only, the results often depend on the timing of the operation. The prognosis is more favorable the earlier the intervention is undertaken.
- Medical genetic counseling
Considering that malformations of the larynx and trachea are a manifestation of embryopathies, in patients with congenital pathologies of these organs, manifestations of embryopathies from other organs and systems are very likely. In clinical practice, the greatest difficulty in establishing the nosological form of the disease is its syndromic forms. The syndromic examination method is based on the fact that most developmental defects can be isolated or be part of known syndromes or unspecified complexes of multiple congenital defects. Establishing a syndromic diagnosis influences the following factors: 1) conducting a thorough diagnosis of hidden developmental defects and functional abnormalities within the established syndrome; 2) performing specific preoperative preparation of the patient to prevent possible complications during surgery or in the postoperative period; 3) tactics and results of treatment, which in some cases is expressed in the refusal of surgical interventions, including changes in the surgical technique for correcting certain developmental defects.
According to our data, a syndromic diagnosis can be established in approximately 25% of patients [4]. Only 8-10% of children have an isolated form of congenital pathology of the larynx and trachea. The remaining patients with congenital diseases of the larynx and trachea have other developmental defects - the central nervous, musculoskeletal, cardiovascular systems, developmental anomalies of the auricles, facial developmental defects, connective tissue abnormalities, congenital tumor-like formations of the skin, etc. A combination of developmental defects of several organs systems that are not induced by each other in this group of patients can be regarded as multiple unspecified congenital malformations.
Literature
1. Bogomilsky M. R., Soldatsky Yu. L., Maslova I. V., Nurmukhametov R. Kh. Congenital juvenile respiratory papillomatosis of the larynx // Bulletin of Otorhinolaryngology. 1998. No. 6. P. 28 - 29. 2. Vodolazov S. Yu., Pospelov N. V. Combined treatment of children with widespread hemangiomatosis of the head, neck, face in combination with subglottic hemangioma of the larynx. In the book: Materials of the XV All-Russian Congress of Otorhinolaryngologists, September 25-29, 1995, Volume II. St. Petersburg, 1995. P. 273 - 275. 3. Gerain V., Chireshkin D. G. Molecular biological aspects of juvenile respiratory papillomatosis and its combined treatment // Bulletin of Otorhinolaryngology. 1996. No. 4. P. 3 - 8. 4. Maslova I.V., Solonichenko V.G., Soldatsky Yu.L., Onufrieva E.K. Genetic aspects of congenital pathology of the larynx and trachea // Bulletin of Otorhinolaryngology. 1999. No. 2. P. 30 - 33. 5. Soldatsky Yu. L., Onufrieva E. K. Subglottic hemangioma as a cause of laryngeal stenosis in young children // Bulletin of Otorhinolaryngology. 1997. No. 6. P. 19 - 21. 6. Soldatsky Yu. L., Maslova I. V., Onufrieva E. K. Laser endoscopic surgery of congenital diseases of the larynx in children // Laser medicine. 1998. T. 2. No. 2 - 3. P. 36 - 38. 7. Soldatsky Yu. L., Onufrieva E. K., Maslova I. V. Stridor in newborns and infants. In the book: Materials of the V Congress of Pediatricians of Russia “Healthy Child”, 02.16-18.1999. Moscow, 1999. P. 430 - 431. 8. Tsvetkov E. A., Fadeeva I. A. Surgical treatment of congenital laryngeal cysts // Bulletin of Otorhinolaryngology. 1999. No. 3. P. 42 - 45. 9. Chireshkin D. G., Onufrieva E. K., Soldatsky Yu. L. Vascular tumors of the larynx, pharynx and oral cavity in children // Bulletin of Otorhinolaryngology. 1994. No. 4. P. 29 - 32. 10. Chireshkin D. G. Chronic obstruction of the laryngeal part of the pharynx, larynx and trachea in children. M.: Rapid-Print, 1994. P. 144. 11. Chireshkin D. G., Maslova I. V., Onufrieva E. K., Soldatsky Yu. L. Structure and early symptoms of congenital diseases of the larynx and trachea // Bulletin otorhinolaryngology. 1996, No. 5. P. 13 - 18. 12. Shanturov A. G., Subbotina M. V. Ultrasound diagnostics in pediatric laryngology. Irkutsk: Papyrus, 1994. P. 140. 13. Avidano MA, Singleton GT Adjuvant drug strategies in the treatment of reccurrent respiratory papillomatosis // Otolaryngology - Head and Neck Surgery. 1995. Vol. 112. P. 197 - 202. 14. Backer CL, Ilbawi MN, Idriss FS Vascular anomalies causing tracheoesophageal compression // J. Thorac Cardiovasc. Surg. 1989. Vol. 97. P. 725 - 731. 15. Bauman NM, Smith RJ Recurrent respiratory papillomatosis // Pediatr. Clin. North. Am. 1996. Vol. 43. P. 1385 - 1401. 16. Belmont JR, Grundfast KM Congenital laryngeal stridor (laryngomalacia): etiologic factors and associated disorders // Ann. Otol. Rhinol. Laryngol. 1984. Vol. 93. P. 430 - 436. 17. Benjamin B., Jacobson I., Eckstein R. Idiopathic subglottic stenoses: diagnosis and endoscopic laser treatment // Ann. Otol. Rhinol. Laryngol. 1997. Vol. 106. P. 770 - 774. 18. Benjamin B., Mair EA Congenital interarytenoid web // Arch. Otolaryngol. Head Neck Surg. 1991. Vol. 117. P. 1118 - 1122. 19. Chmielik M., Piekarniak P., Snieg B. Microsurgical treatment of laryngeal papillomatosis // Otolaryngol. Pol. 1997. Vol. 51. P. 26 - 30. 20. Civantos FJ, Holinger LD Laryngoceles and saccular cysts in infants and children // Arch. Otolaryngol. Head Neck Surg. 1992. Vol. 118. P. 296 - 300. 21. Deunas L., Alcantud V., Alvarez F. et al. Use of interferon-alpha in laryngeal papillomatosis: eight years of the Cuban national program // J. Laryngol. Otol. 1997. Vol. 111. P. 134 - 140. 22. Ferguson CF Congenital abnormalities of the infant larynx // Ann. Otol. Rhinol. Laryngol. 1967. Vol. 76. P. 744 - 752. 23. Friedman EM, Vastola AP, McGill TJ, Healy GB Chronic pediatric stridor: etiology and outcome // Laryngoscope. 1990, Vol. 100. P. 277 - 280. 24. Froehlich P., Seid AB, Morgon A. Contrasting strategic approaches to the management of subglottic hemangiomas // Int. J. Pediatr. Otorhinolaryngol. 1996. Vol. 36. P. 137 - 146. 25. Gonzales C., Reilly JS, Bluestone CD Synchronous airway lessions in infants // Ann. Otol. Rhinol. Laryngol. 1987. Vol. 96. P. 77 - 80. 26. Grundfast KM, Harley EH Vocal cord paralysis // Otolaryngol. Clin. North. Am. 1989. Vol. 22. P. 569 - 597. 27. Healy GB, McGill T., Friedman EM Carbon Dioxide Laser in Subglottic Hemangioma. An update. //Ann. Otol. Rhinol. Laryngol. 1984. Vol. 93. P. 370 - 373. 28. Holinger LD Etiology of stridor in the neonatal, infant and child // Ann. Otol. Rhinol Laryngol. 1980. Vol. 89. P. 397 - 400. 29. Holinger LD, Holinger PC, Holinger PH Etiology of bilateral abductor vocal cord paralysis: A review of 389 cases // Ann. Otol. Rhinol. Laryngol. 1976. Vol. 85. P. 428 - 436. 30. Holinger LD, Lusk RP, Green CG Pediatric laryngology and bronchoesophagology. Philadelphia - NY: Lippincott - Raven, 1997. R. 402. 31. Holinger PH, Brown WT Congenital webs, cysts, laryngoceles and other anomalies of the larynx // Ann. Otol. Rhinol. Laryngol. 1967. Vol. 76. P. 744 - 752. 32. Jacobs I., Welmore R., Tom L. et al. Tracheobronchomalacia in children // Arch. Otolaryngol. Head Neck Surg. 1994, Vol. 120. P. 154 - 158. 33. McGill T. Congenital diseases of the larynx // Otolaryngol. Clin. North. Am. 1984. Vol. 17. P. 57 - 62. 34. Miller R., Gray SD, Cotton RT, Myer CM, Netterville J. Subglottic stenosis and Down syndrome // Am. J. Otolaryngol. 1990. Vol. 11. P. 274 - 277. 35. Myer CM, Cotton RT, Holmes D. Laryngeal and laryngotracheoesophageal clefts: The role of early surgical repair // Ann. Otol. Rhinol. Laryngol. 1990. Vol. 99. P. 98 - 104. 36. Nowlin JH, Zalzal G. The stridorous infant // ENT J. 1989. V. 70. P. 84 - 88. 37. Park SC Vascular abnormalites // Pediatr. Clin. North. Am. 1981. Vol. 28. P. 949 - 955. 38. Park SS, Streitz JM Jr., Rebeiz EE, Shapshay SM Idiopathic subglottic stenosis // Arch. Otolaryngol. Head Neck Surg. 1995. Vol. 121. P. 894 - 897. 39. Parnell FW, Brandenberg JH Vocal cord paralysis: A review of 100 cases // Laryngoscope. 1970. Vol. 70. P. 1036 - 1045. 40. Pransky SM, Grundfast KM Differentiating upper from lower airway compromise in neonates // Ann. Otol. Rhinol. Laryngol. 1985. Vol. 94. P. 509 - 515. 41. Richardson MA, Cotton RT Anatomic abnormalities of the pediatric airway // Pediatr. Clinic. North. Am. 1995. Vol. 31. P. 821 - 834. 42. Rimmell FL, Stool SE Diagnosis and management of pediatric tracheal stenosis // Otolaryngol. Clin. North. Am. 1995. Vol. 28. P.809 - 827. 43. Shikhani AH, Marsh BR, Jones MM, Holliday MJ Infantile subglottic hemangiomas. An update // Ann. Otol. Rhinol. Laryngol. 1986. Vol. 95. P. 336 - 347.
Note!
- Stridor in newborns is a symptom of partial obstruction of the large diameter airways
- To diagnose the disease, a thorough history and clinical examination of the child is necessary to assess the severity of his condition.
- The level of damage can be suspected by the stridor phase and associated symptoms, such as cough, regurgitation, cyanosis
- The main method of diagnosis is endoscopy, although radiographic and ultrasound examinations can be very useful in some cases
- All patients with congenital pathology of the larynx and trachea need to be examined in a medical genetic consultation
Treatment options
The inflection of the bile duct does not go away asymptomatically
Treatment of defects formed in the structure of the bile reservoir is carried out mainly by conservative methods. The doctor must prescribe to the patient special medications that have a predominant choleretic effect in the body, as well as various types of antispasmodics that prevent excessive accumulation of bile in the body. Physiotherapeutic methods are also widely used. Special procedures prescribed by the attending physician are aimed at improving blood flow to the organ and restoring the activity of all existing muscles, as well as promoting their normal functioning.
In many cases, the child is prescribed to visit sanatoriums and resorts in order to increase the effectiveness of treatment.
The sick child is prescribed a special diet. Usually, high-fat, fried, and spicy foods are excluded from the daily menu. There is no need to pamper your child with an abundance of sweets and confectionery. Also, do not overuse flour products and various baked goods.