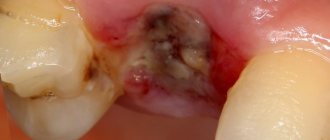
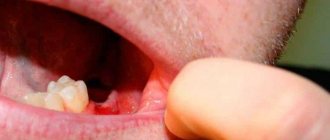
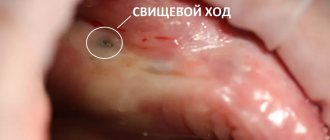
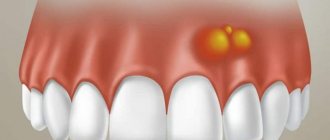
The doctor makes the diagnosis of “post-extraction alveolitis” based on a visual examination. To confirm the diagnosis, X-ray diagnostics is prescribed. An x-ray can show changes in tissue, identify tooth fragments, a cyst or granuloma, which could cause inflammation.
The final result of treatment of alveolitis should be:
- Elimination of inflammation;
- Cleaning the hole from foreign bodies;
- Complete healing of the hole;
- Exclusion of the development of complications.
Treatment at the dentist
The doctor begins treatment by washing the socket and treating it with antiseptic solutions, and then cleans the socket from the remains of the blood clot using a surgical curette. Then the wound is dried with a gauze swab and treated with an anesthetic and antibacterial agents. The wound is covered with a bandage, which is designed to protect the open surface of the wound from possible biological, chemical or mechanical irritants. To check the possibility of detecting pieces of the extracted tooth in the socket, an x-ray can first be taken.
The procedure for cleaning the hole as a whole is carried out according to the following scheme:
- Local anesthesia is performed;
- The well is washed with an antiseptic solution (hydrogen peroxide solution 3%, chlorhexidine 0.05% or furatsilin 0.02%), and food debris and necrotic masses are removed;
- If there are foreign bodies in the hole (root fragments, cysts and granulomas), they are removed using special instruments;
- After cleaning the hole, it is treated with antiseptic solutions, dried with a sterile gauze swab, and turunda with an antiseptic and an anesthetic is injected into it. With a mild degree of inflammation, a turunda may not be necessary; thorough cleansing of the hole and subsequent care for it is sufficient;
- In case of a pronounced necrotic process in the hole, rinsing and application with trypsin is carried out - this is an enzyme preparation that accelerates the breakdown of dead tissue. Trypsin has anti-inflammatory and anti-edematous effects, helps clean the socket from necrotic masses and pus;
- After completing all the manipulations, the patient goes home, the doctor appoints appointment days when he needs to come for antiseptic treatment of the hole and change the turunda, if one has been installed. If necessary, a course of antibiotics is prescribed.
For alveolitis, antiseptic baths (not rinsing) with solutions of chlorhexidine 0.05% or miramistin 0.01%, which can be purchased ready-made at the pharmacy, are effective. When performing baths, the solution is taken into the mouth and held for several minutes, then carefully spat out. To relieve pain and reduce the degree of inflammation, nimesulide or ibuprofen are prescribed.
To prevent the turunda from falling out of the socket, during treatment you need to eat soft, pureed food and do not chew on the sore side. If the turunda does fall out, you need to rinse your mouth with chlorhexidine solution and immediately consult a doctor.
If this is not possible, you should rinse the hole yourself from food debris: to do this, bite off the sharp tip of the needle from a 5 ml syringe, bend it a little, and disinfect it with pure alcohol. A chlorhexidine solution is drawn into the syringe, the needle is inserted into the hole (not too deep) and the piston is pressed intensely to create a liquid pressure that can remove food debris.
All cases of alveolitis treatment are individual, so it may be necessary to visit the dentist up to several times.
With a favorable course of the healing process, the pain goes away, and the inflammatory process gradually subsides and disappears after a few days.
If the process, despite the procedures performed, progresses, then after antiseptics, gauze tampons soaked in propolis tincture or camvorophenol solution (10%) are inserted into the hole. A tetracycline-prednisolone cone inserted into the well has a good antibacterial effect.
Treatment of alveolitis
Treatment of alveolitis, regardless of its etiology, is a very difficult task, the solution of which clearly requires professional medical care. In no case should you act independently and at home, because with an illiterate approach there is a high chance of causing significant harm.
Conditionally, the treatment of alveolitis can be classified into stages - depending on how timely the alveolitis was diagnosed, the treatment and general management tactics are determined.
Early treatment
If alveolitis was diagnosed in the initial stages, then to get rid of the disease it is sufficient to perform the following measures:
- The implementation of drug anesthesia is primarily because, despite its relative simplicity, the process of getting rid of alveolitis is quite painful.
- Treatment of the hole in which there is an inflammatory process is washed with an antiseptic solution.
- Removing necrotic debris from the socket.
- Repeated treatment of the hole with an antiseptic followed by drying with gauze.
- Placement on top of fabric soaked in antiseptic and drugs that provide an anesthetic effect.
- Apply applications with antiseptics daily (for a week) in order to eliminate the possibility of a relapse of the inflammatory reaction.
Procedures for continuing treatment at home
Treatment of alveolitis at home is carried out when acute symptoms have been eliminated, antiseptic turundas are no longer needed and the goal is to speed up the healing of the hole. For this use:
- Mouth rinses with infusions of chamomile, calendula, and sage. These medicinal plants have anti-inflammatory properties and accelerate healing processes. Rinsing is carried out several times during the day, always after meals.
- Applications with dental adhesive paste Solcoseryl. The drug belongs to the group of tissue regeneration stimulators: it accelerates healing, improves the supply of cells with oxygen and nutrients. The paste has a pleasant mint taste and contains the anesthetic component polidocanol 600. To properly apply the paste, you need to dry the hole with a gauze swab and fill it with Solcoseryl, lightly moisten the paste with water on top. The procedure is repeated several times a day as necessary; the paste is able to protect the socket throughout the day from mechanical and chemical influences.
- Taking vitamin preparations. You can purchase any vitamin and mineral complex at the pharmacy (Vitrum, Duovit, Complivit); Vitamins are taken to increase the body's defenses and shorten the recovery period.
Results and discussion
When analyzing patient complaints, the first place was occupied by the pain symptom. In all patients who took part in the study, pain of varying characteristics (sharp, twitching or aching) in the socket, which arose on the 2-3rd day after tooth extraction, was the main reason for visiting a dentist; the second place among the complaints was presence of bad breath. At the same time, the majority of patients did not note any disturbance in their general condition; in both groups, when measuring body temperature, it was within the subfebrile range, which indicated the absence of pronounced systemic changes requiring antibiotic therapy.
During control examinations of patients on the 3rd day: in group 1, the majority of patients (60%, n
=9) still noted the pain symptom as severe, the remaining participants (40% (
n
=6)) - as moderate. All patients of group 1 noted an unpleasant taste of iodine in the mouth and bad breath, which is directly related to the use of iodoform turunda. During examination, the turunda was in place in all cases; food contamination of its upper layer was noted. The edges of the wound in all cases were hyperemic and swollen. The replacement of the turunda was carried out according to the standard method, but no additional antiseptic treatment was performed.
In the 2nd group with the drug Cholisal, only 5 patients noted a pronounced pain reaction, 6 noted moderate pain, and the remaining 4 patients did not note any pain on the 3rd day from the start of using the drug. Complaints of an unpleasant taste in the mouth were noted by only 20% ( n
=3).
When examining the socket of the extracted tooth, 80% ( n
= 12) of patients were noted to be filled with gel without signs of foreign contamination. This fact can be explained by the mode of administration of the drug - 4 times a day, after preliminary rinsing with water if necessary, which makes it possible to eliminate possible food debris. When interviewing patients, no difficulties with self-administration of the drug were identified.
On the 5th day, patients of group 1 with iodoform turunda noted a pronounced pain reaction in 6 cases, moderate pain in 5 cases, and only 4 patients did not have pain complaints during the last day. Complaints about taste and odor from the mouth still persisted in all patients of group 1, which could be due to significant contamination of the upper layer of the turunda with food debris and plaque. During this visit, the turunda was also replaced with a new one without additional antiseptic treatment. During the dressing, the formation of epithelium on the inner side of the mucous socket, expressed to varying degrees, was noted in all patients.
In group 2, where Cholisal was used, the dynamics of subjective sensations were much more pronounced - only 5 patients noted slight discomfort in the area of the extracted tooth socket, and the remaining 10 did not note any pain or other sensations for at least the last 2 days. There were no complaints about organoleptic properties during this period. Upon examination, the sockets in all patients were filled with gel without foreign impurities; there was a pronounced convergence and epithelization of the edges of the wound, and a decrease in the mouth of the socket. The surrounding mucosa retained slight swelling and hyperemia only in 2 cases.
Due to the lack of objective tools for measuring pain symptoms, we focused on laboratory parameters to assess the effectiveness of treatment. However, complaints and results of clinical examination were recorded at each follow-up visit.
When analyzing biochemical parameters before treatment in patients diagnosed with alveolitis, the content of PI in the blood differed from the corresponding indicators in healthy individuals [5]. This, in turn, naturally led to a change in the concentration of AA, one of the main products of metabolism of P.I. Analysis of PGE2 content also revealed a significant increase in indicators compared to healthy individuals (Table 1).
Table 1. Biochemical parameters of inflammatory markers before treatment Note. 1 - see the list of references, paragraph 4. * - the differences in indicators in healthy individuals and patients diagnosed with “alveolitis” of the “dry socket” type are significant (p <0.05). Thus, the local inflammatory reaction in the mouth is reflected at the systemic level, which made it possible to use these parameters to objectify the assessment of the use of the drug Cholisal in the treatment of patients diagnosed with alveolitis.
Analysis of biochemical parameters in patients with alveolitis on the 5th day after the start of treatment showed that the content of PI, AA, and PGE2 in whole gingival blood significantly decreased compared to the initial level in both clinical groups (Table 2).
Table 2. Biochemical parameters of inflammatory markers on day 5 Note. 1 - see the list of references, paragraph 4. * - the differences in indicators in healthy individuals and patients of groups 1 and 2 are significant (p <0.05). However, a more pronounced, statistically significant decrease in indicators was observed in group 2, where patients were prescribed the drug Cholisal. During this period, satisfactory clinical regeneration of the tooth socket had not yet occurred, however, biochemical parameters had a pronounced positive trend. Probably, these data on the level of PI, AA, PGE2 in patients of group 2, in contrast to patients of group 1, are explained by the anti-inflammatory effect of the drug Cholisal. The obtained biochemical parameters fully correlated with the subjective data of the patients during control examinations.
During the control examination on the 10th day in the 1st group with iodoform turunda, when collecting complaints, only 4 patients noted slight discomfort in the area of the extracted tooth socket, and the remaining 11 did not note any pain during the last day. At this stage, the main complaint of patients was an unpleasant taste and odor from the mouth. Clinical examination revealed the absence of swelling and hyperemia of the mucous membrane near the hole in all patients, however, in all cases, contamination of the upper layer of the turunda was still noted.
In group 2 with Cholisal, by this time patients did not show any complaints. Upon examination, the edges of the socket were epithelialized in 100% ( n
=15) cases, in 80% (
n
=12) of patients the edges were brought as close as possible, but a gap was maintained for drug administration.
Analysis of biochemical parameters, carried out on the 10th day from the start of treatment, showed a correlation with clinical examination data and revealed the high effectiveness of local use of the drug Cholisal in the treatment of alveolitis. Thus, all the studied biochemical indicators in group 2 were at the level of normal values or had a slight difference, while in patients of group 1 the indicators still exceeded the normal level for all studied positions (Table 3).
Table 3. Biochemical parameters of inflammatory markers on the 10th day Note. 1 - see the list of references, paragraph 4. * - the differences in indicators in patients with alveolitis before and after treatment are significant (p <0.05).
Based on the data of clinical examinations and the subjective sensations of patients, the reduction or complete elimination of the pain symptom and inflammatory component occurred 2-2.5 times faster in the group of patients who used Cholisal, compared to the group of standard methods of alveolitis management. This also applies to indicators of biochemical processes - their dynamics in the group with Cholisal were better on all points and correlated with clinical data (Tables 4, 5,
Table 4. Dynamics of biochemical parameters on the 5th day from the start of treatment
Table 5. Dynamics of biochemical parameters on the 10th day from the start of treatment Fig. 2, 3).
Rice. 3. Dynamics of PGE2 indicators on the 5th and 10th days by group. Fig. 3. Dynamics of prostoglandin E2 indices on the 5th and 10th days by groups.
Rice. 2. Dynamics of FI indicators on the 5th and 10th days by group.
Summing up the results of the study, it should be noted that the dynamics of subjective sensations towards improvement in patients of group 2 compared with those in group 1 already on the 3rd day from the start of treatment and further throughout the entire period, in our opinion, is associated with a pronounced analgesic and antiseptic effect of the drug Cholisal. Local administration of the gel promotes a direct effect on the site of inflammation by suppressing the synthesis of cyclooxygenase and prostaglandins responsible for the reaction cascade. When surveyed, the biggest advantages were cited by study participants as the rapid onset of an analgesic effect and the ability to use Cholisal at home, which makes the procedure more convenient, although it requires prior training. However, none of the patients experienced any difficulties with self-administration of the drug.
The gel form promotes long-term stay in the injection zone, which was noted by patients. From the point of view of clinicians, this effect helps to prolong the drug effect on the socket, which is undoubtedly a big plus.
Thus, based on an analysis of the clinical course, subjective indicators (patient complaints, ease of self-administration) and biochemical research data when using the drug Cholisal for the treatment of alveolitis, which occurs as a “dry socket”, its effectiveness has been established, which is not inferior and even has advantages in comparison with the classical method of managing patients in the treatment of this nosology.
Additional physiotherapy treatment (click to expand)
Physiotherapeutic treatment is an important addition to drug therapy; with the help of physiotherapy, the intensity of inflammation can be significantly reduced and healing time can be accelerated. For alveolitis, the following techniques are used:
- UV therapy - the hole is irradiated with short-wave ultraviolet light, which kills pathogenic microorganisms and reduces the level of inflammation.
- SMV therapy is a method of treatment with an electromagnetic field, based on the effect of centimeter waves on the area of inflammation. The procedure helps improve blood circulation and metabolism, due to which toxic substances are removed from tissues faster and regeneration processes are accelerated. SMV therapy also has an analgesic effect.
- UHF therapy – the body is exposed to a high-frequency electromagnetic field. For alveolitis, UHF therapy is used if the patient's regional lymph nodes are enlarged.
- Electrophoresis – medications are injected into inflamed tissue using electrical impulses. For post-extraction alveolitis, electrophoresis is used to reduce pain. For this purpose, solutions of novocaine, lidocaine, trimecaine are used.
- Fluctuarization is a treatment technique with pulsed currents of a sinusoidal shape with a low frequency. As a result of the procedure, blood circulation and lymph flow improves, swelling resolves, and the level of inflammation decreases.
- Laser therapy - the hole is exposed to infrared laser radiation, which has an anti-inflammatory effect, reduces swelling and redness of soft tissues, and accelerates healing.
Complications of alveolitis
If alveolitis is not treated in a timely manner, the following complications may develop:
- Odontogenic sinusitis is an inflammation of the maxillary sinus caused by the spread of infection from the inflamed sockets after the removal of premolars or molars of the upper jaw;
- Phlegmon - purulent inflammation spreads to the surrounding soft tissues;
- Acute periostitis - pus accumulates in the periosteum area;
- Odontogenic osteomyelitis is a purulent-necrotic lesion of the jaw bone;
- Sepsis - an infection enters the bloodstream, causing it to become infected.
Alveolitis itself is not so dangerous, but its complications are life-threatening. Therefore, if you notice symptoms of alveolitis, contact your doctor immediately.
The patient's role in the prevention of alveolitis
According to statistics, in most cases, the cause of the development of post-extraction alveolitis is the patient’s incorrect actions after tooth extraction, ignoring the recommendations of the attending physician. After tooth extraction it is prohibited:
- Remove the blood clot from the socket. The blood clot that forms in the hole after tooth extraction prevents microbes from entering the wound, and the healing process under it proceeds quickly and without complications. Patients can remove the clot by touching it with the tongue, with fingers, by vigorously rinsing the mouth immediately after tooth extraction, and also while eating solid foods.
- Do hard physical work, sports, take hot baths, go to the sauna. Intense loads and elevated temperatures provoke the opening of the wound, and bleeding resumes; pathogenic microorganisms can enter the wound.
- Smoking, drinking alcohol. Bad habits lead to excessive irritation of the mucous membranes, healing of the hole is much slower, and inflammation may occur.
To speed up healing and prevent the development of inflammation in the socket, you need to:
- In the first few days after tooth extraction, review your menu, excluding spicy, too salty, sour, and hot dishes. All food should be soft, pre-chopped;
- Maintain careful oral hygiene. The presence of chronic inflammation of the gums and carious teeth in the mouth can cause infection of the socket, so after tooth extraction you need to carry out antiseptic baths (they should be prescribed by a doctor);
- After each meal, rinse your mouth with clean water to remove any remaining food; this must be done very carefully so as not to remove the blood clot covering the hole;
- Brush your teeth carefully, trying not to touch the socket with the brush.
Causes of the disease
The development of the disease can be caused by many reasons, from violation of the treatment regimen to serious pathologies. The most common factors:
- Excessively frequent mouth rinsing. Causes blood to be washed out of the socket, facilitating the penetration of bacteria there;
- The entry of food into the hole, which, if cleaned poorly, causes an inflammatory process;
- Low immunity, lack of vitamins, minerals and trace elements in the body;
- Complications after surgery;
- During the operation, oral hygiene was poor; dental plaque got there and was not removed.
Symptoms
The first and main sign of the disease is that the socket in place of the extracted tooth does not heal. If blood constantly oozes out at the removal site, then the formation of a protective blood clot is disrupted and the situation needs to be corrected. Remember, an open wound is not protected from bacteria, so unwanted inflammation can begin there at any moment. When this process occurs, purulent discharge and bad breath appear. It is important not to self-medicate, but to consult a doctor to adjust treatment.
The role of the doctor in excluding the possibility of alveolitis
Actions of the dental surgeon to exclude alveolitis:
- Thoroughly clean the socket so as not to leave a tooth fragment or cyst in it. After extracting a tooth, especially a damaged one, a control x-ray of the socket is often taken;
- Be careful and avoid injury. The tooth extraction was accompanied by bone injury due to the inept actions of the doctor. Usually the bone is injured during complex extraction, when tooth extraction cannot be carried out using conventional instruments. Difficult procedures include the removal of unerupted and incorrectly positioned wisdom teeth, multi-rooted teeth, and teeth with curved or destroyed roots. An inexperienced doctor may not understand the situation and damage the bone;
- Control during anesthesia. An overdose of anesthetic leads to a sharp decrease in the amount of blood released after tooth extraction and insufficient formation of a blood clot;
- Prescribing appropriate antibacterial drugs, especially if the tooth extraction was difficult or was carried out against the background of purulent inflammation.
Therefore, it is very important to seek help from competent and experienced specialists who are fully familiar with all the intricacies of the tooth extraction procedure.
Sometimes alveolitis can develop despite preventive measures taken due to certain reasons. These reasons include:
- Reduced immunity of the patient, inability of tissues to regenerate;
- Tendency to bleed, resulting in a blood clot not forming;
- An increase in the amount of the hormone estrogen in women when taking hormonal contraceptives or certain diseases, which leads to the destruction of a blood clot.
A timely visit to the dentist if alveolitis develops is the key to a quick cure. Patients of our clinic who have undergone tooth extraction surgery receive detailed recommendations on oral care; if they are strictly followed, the likelihood of developing alveolitis is excluded.