The main task of a dental surgeon during the treatment of a fracture of the upper or lower jaw is to restore the anatomical structure of the broken bone and the correct relationship of the dentition. Many techniques help to achieve this, but the effectiveness of treatment also depends on how correctly and quickly first aid was provided.
Before hospitalization
First aid to the victim includes:
- stopping bleeding (pressing or packing the wound, applying cold);
- if necessary, cardiopulmonary resuscitation;
- pain relief (analgin, revalgin intramuscularly);
- immobilization of the jaw with the help of fixing bandages (contraindicated if the victim is unconscious, since this increases the risk of suffocation from the retraction of the tongue or vomit entering the respiratory tract).
Osteosynthesis
Indispensable for complex, comminuted and multiple fractures with displacement, loose teeth and complete absence of teeth, for periodontal disease and other inflammatory diseases of the gums in the area of injury. Osteosynthesis is also effective in cases of fracture of the condylar process complicated by dislocation of the articular head of the lower jaw.
Fastening materials can be steel knitting needles and rods, pins, nitride-tinan wire with shape memory, quick-hardening plastics, polyamide thread, special glue.
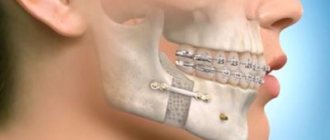
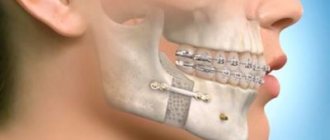
However, osteosynthesis with metal miniplates is considered the most convenient and safe method today. They allow you to cut through the skin and muscles on only one side, which simplifies the operation itself and shortens the recovery period. Another undeniable advantage is the ability to reliably fix fragments in areas with significant dynamic loads.
Possible consequences
A bruise is not usually considered a serious injury. However, if you neglect the necessary treatment, unpleasant consequences arise. For example, the result of a bruise of the lower jaw can be a violation of the depreciation of muscle fibers, changes in the cartilage tissue of the joint and a speech defect.
On the muscle side, post-traumatic myositis develops as a complication. It is an inflammatory process, which is subsequently difficult to respond to therapeutic effects.
Attention!!! Bruises of various etiologies often become the cause of the formation of oncological tumors. Timely diagnosis and proper treatment can completely eliminate this complication.
With insufficient attention to the problem, jaw deformation, post-traumatic periostitis and even osteomyelitis occur. Abscesses and phlegmons may form in soft tissues. Such conditions require long-term therapy, with a long recovery period.
Injury to the maxillofacial area is not a trivial matter. It is worth treating this problem with increased attention. Of course, many of them go away on their own. However, ideally any injury should be examined by a medical professional.
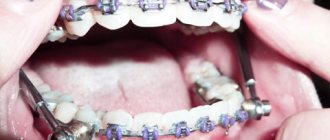
Splinting the jaw
This is the immobilization (fixation) of bone fragments using a special plastic or wire structure.
The technique, created by military doctors at the beginning of the 20th century, is successfully used by dentists today. The materials used to make the splint have changed, and the methods of applying it have been improved.
Today, a specialist has many types of tires in his arsenal:
- from standard Vasiliev tape splints, the simplest and cheapest method of treatment;
- to aluminum Tigerschdedt splints, which are made individually for each patient, due to which they are more effective. In addition, they evenly distribute the load and minimally injure the teeth.
The type of splinting depends on the type of injury and can be unilateral (when one jaw is fractured) or bilateral (when both are damaged).
If the teeth are preserved, it is not difficult to apply a bent dental wire splint. It is bent to the shape of the dental arch and fixed with bronze-aluminum wire ligatures, which, like a hairpin, cover the tooth on both sides. Manipulations are performed under local anesthesia.
When both jaws are fractured, a structure with a more rigid base is installed; in addition to wire, hooks and rings are also used that immobilize the lower jaw.
International standards
A real revolution in maxillofacial surgery occurred in 1958, when M. Muller, M. Allgower, R. Schneider, H. Willenegger organized the International Association for the Study of Internal Fixation (AO/ASIF - Ardeitsgemeinschaft fur Osteosynthesefragen/Association for the Study of Internal Fixation – working association for the study of osteosynthesis/association for the study of internal fixation).
According to the postulates of AO/ASIF, the osteosynthesis technique implies that:
1. the structures used must be made of bioinert metal alloys;
2. bone fragments must be anatomically accurately compared and fixed;
3. the use of gentle surgical techniques ensures the preservation of blood supply to bone fragments and surrounding soft tissues;
4. stable fixation of fragments is ensured by interfragmentary compression;
5. early application of functional load is indicated;
6. restoration of contractile activity of muscles and movement in the joint.
AO/ASIF staff also developed and implemented metal plate systems for mandibular osteosynthesis:
· dynamic compression plates;
· reconstructive (blocking) plates (Locking reconstruction plates);
· blocking (locking) plates (Locking plates 2.0 mm);
· universal plates (Universal fracture plates);
· mandibular plates (Mandible (Mandible plates 2.0 mm).
They developed dynamic compression plates (DCP), through which it was possible to create compression between fragments for their primary fusion. The design of these plates includes oval holes with beveled walls, which allows the fragments to be brought closer together when the screws are tightened. The use of dynamic compression plates made it possible to achieve stable internal immobilization, reduced the number of cases of delayed fusion of fragments, and eliminated the need for additional fixation. But their use still does not eliminate the risk of microcracks in the area of the fracture line and the development of osteoporosis in the bone at the site of contact with the plate.
The locking plate/screw system, with threaded plate holes and locking screw heads, was developed to prevent bone necrosis under the plate. The system provides rigid fixation of bone fragments using a plate and a plate and screws to each other - this helps prevent the screws from unscrewing and avoid possible displacement of the fragments while tightening the screws in the hole of the plate. The plate itself is located at a certain distance from the surface of the bone, which prevents the development of lysis.
Foreign studies have not revealed significant differences in the effectiveness and possible development of postoperative complications during osteosynthesis with locking plates with screws and non-locking plates.
Another system developed by AO/ASIF experts is the LCP (locking compression plate system with angular stability) is a design of multi-cell plates with numerous holes and consists of two parts: a threaded one for fixing the head of a locking screw and a hole for creating dynamic compression by eccentric insertion of standard cortical or cancellous screws.
Installation of the plate requires special tools and is carried out according to clearly established technology.
If the adjustment of the LCP to the shape and relief of the outer surface of the lower jaw bone is carried out in accordance with the established requirements, then this creates ideal conditions for the fusion of fragments during osteosynthesis of multiple comminuted fractures of the lower jaw of various locations, in case of suppuration of a bone wound, traumatic osteomyelitis, in case of a fracture with the occurrence of a bone defect tissue, fracture of toothless jaws. Limited contact of LCP with bone helps prevent the development of bone necrosis under the plate.
Is it possible to do without splinting?
Even if the case is not severe - the fracture is one-sided, closed and without displacement - it is imperative to take measures to prevent the development of such unpleasant complications as:
- accidental displacement of fragments,
- re-injury
- development of inflammation of soft tissues,
- infection of the fracture site.
To do this, it is necessary to immobilize the jaw by any available method. This can be a sling bandage, but it is much more convenient and effective to use a splint. In case of a complicated fracture, splinting is absolutely indispensable, regardless of the location of the injury.
Treatment tactics for displaced fractures
In such cases, before applying a splint, it is necessary to compare the jaw fragments, for which reduction orthopedic devices are used. A broken upper jaw requires traction using special dental splints.
Such injuries are very dangerous because they can cause asphyxia. But correctly provided first aid will prevent suffocation. Clear the oral cavity of foreign bodies or blood, lay the victim face down, placing a cushion rolled up from clothes, blankets, etc. up to the chest.
Rehabilitation after a jaw fracture
For successful treatment of a jaw fracture, anti-inflammatory and restorative therapy, physiotherapy, mechanotherapy and special oral hygiene are also important.
- Within 3-4 days after the injury, antibiotics must be prescribed to prevent inflammation, which are injected directly into the area of injury.
- General strengthening therapy is taking vitamins C, P, D and group B, drugs that stimulate tissue regeneration and restore the level of leukocytes in the blood.
- Among the effective physical procedures, we note UHF therapy, general ultraviolet irradiation, and magnetic therapy. After the third procedure, swelling and pain are noticeably reduced, swelling subsides. For better healing of fragments, 2 weeks after a jaw fracture, electrophoresis is performed using a two to five percent solution of calcium chloride.
- Mechanotherapy, or physical therapy, accelerates the restoration of jaw function and helps if, after an injury, the mouth opens poorly or does not open at all. It can also be practiced at home, starting 4-5 weeks after the fracture, when the splints are removed and a callus has formed.
- Special hygiene involves irrigation at least 8-10 times a day. For unconscious victims, their teeth and mucous membranes are treated with a special solution at least twice a day.
Diagnostic measures
If minor injuries to the maxillofacial area occur, they do not require contact with a dentist or surgeon, or urgent hospitalization. If there is severe and prolonged pain, the area of damage should be examined by a specialist.
The following are used as diagnostics:
- taking anamnesis;
- general examination by a surgeon, orthopedic dentist, traumatologist;
- special examination by an otolaryngologist, neurologist and other specialized specialists as necessary;
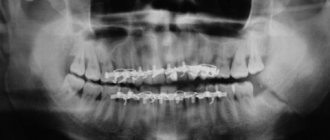
- X-ray examination of the maxillofacial area;
- CT scan;
- analysis of blood, urine, saliva.
Based on the data obtained, a general picture of the victim’s health is formed and a specific treatment is recommended.
The main therapeutic direction will be the following:
- taking painkillers;
- applying a pressure bandage;
- ensuring maximum peace for the victim;
- prescription of physiotherapeutic procedures;
- local and general anesthesia;
- elimination of hematoma and infiltrate.
How to eat?
Since during intensive therapy and during the recovery period the jaws are rigidly fixed and habitual chewing of food is out of the question, correction of the diet is necessary during this period.
Food should have the consistency of low-fat sour cream. These are broths, pureed soups, carefully chopped vegetables and fruits, milk drinks, liquid cereals. Spices are excluded, salt consumption is limited. The temperature of the dish should not be higher than 45-50 °C. The most convenient way to eat food is through a straw.
You need to gradually switch to your usual diet after removing the splint. This is important not only for restoring chewing functions, but also for preventing disorders in the gastrointestinal tract.
Purpose of the operation
When performing an operation, the surgeon sets himself the following goals:
- Combine the fragments;
- Fix the bone with special splints until its integrity is restored;
- Secure the fragments with metal plates and knitting needles;
- Fix the dentition with special structures;
- Create conditions for favorable bone healing.
If such goals are achieved using conservative methods, then there is no need for surgery. Disturbances in the bone structure also cannot be ignored. Otherwise, unpleasant changes develop that lead to impaired chewing and articulation, as well as chronic pain in the jaw.
How much does it cost to treat a broken jaw?
The price depends on the nature of the injury, whether osteosynthesis was performed, what splints were used, and whether the patient attended physical therapy procedures. But let's say for sure that the service is not cheap. Osteosynthesis alone will cost from 14,000 to 55,000 rubles.
It is also necessary to consider the cost of subsequent dental treatment to restore lost teeth or damaged teeth after splinting. Our service will help you choose a competent specialist and not waste your money. Compare prices and services of different clinics, read reviews from real patients.