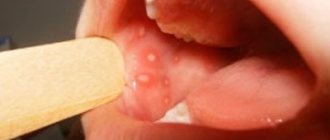
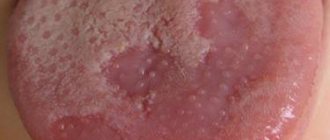
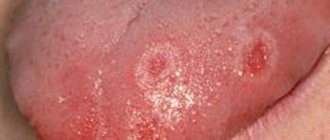
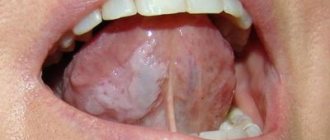
Oral lichen planus, or stomatodermatosis , is a chronic disease of the oral cavity. It is characterized by abundant formation of papillomas, plaques and erosions in the oral cavity, accompanied by inflammatory and degenerative damage to the oral mucosa. This is one of the most common pathologies of the oral cavity, affecting the back of the cheeks, gums, lips, tongue and surface of the hard palate. The likelihood of this disease occurring largely depends on the individual predisposition of the patient. The disease is not transmitted by contact.
Causes of the disease
Lichen planus occurs under the influence of a number of factors, among which the most common is immuno-allergic. When the body's immunity decreases under the influence of external and internal factors, T-lymphocytes cannot cope with their protective function.
Factors that provoke the development of oral lichen planus include:
- Chronic stress;
- Strong shocks;
- Diseases of the gastrointestinal tract;
- Diabetes;
- Hypertension;
- Grynszpan syndrome;
- Injuries to the oral mucosa;
- Incorrectly installed dentures;
- Fillings that injure the oral mucosa;
- Prostheses made of dissimilar materials;
- Long-term use of tetracycline;
The risk group also includes patients whose work involves developing camera film or who come into contact with paraphenyldiamine.
Lichen planus
Lichen ruber planus, described by Wilson in 1869, is a chronic inflammatory disease characterized by monomorphic papules on the skin and visible mucous membranes, most often on the oral mucosa and red border of the lips, accompanied by itching of varying severity. Today, this disease remains an urgent problem associated with the constant frequency of its detection, the lack of a unified pathogenetic concept, as well as the presence of severe forms and a chronic course, often resistant to therapy [1, 4, 6, 13]. In the general structure of dermatological morbidity, lichen planus (LP) accounts for 0.78–2.5%, among diseases of the oral mucosa - 35%. This disease occurs in all races, in all age groups and in both sexes, although the mucous membrane is more often affected in women from 40 to 60 years of age [1, 19].
Etiology and pathogenesis. In modern literature, various theories of the development of LP can be traced, such as viral, neurogenic, hereditary, intoxication and immunoallergic [1, 10, 15, 17].
The immunoallergic theory of the development of this pathology, based, according to various authors, on a decrease in the number of T cells in the patient’s blood and their functional activity, deserves the most attention at present. Some authors have shown a decrease in T-helper cells and an increase in the T-helper/T-suppressor ratio [11–14].
On the oral mucosa, manifestations of LP are associated with the presence of pathologies in patients with the gastrointestinal tract (gastritis, colitis, etc.), liver, and pancreas. Also, in a number of patients there is an undoubted connection between the development of the disease and vascular (hypertension) and endocrine (diabetes mellitus) pathology. Trauma to the oral mucosa, including those caused by dental pathology, has a certain significance in the development of the disease on the oral mucosa: sharp edges of teeth, poorly fitted removable plastic dentures, missing teeth, etc. [1, 6, 7].
Recently, there have been increasing reports of the development of lichen planus of the skin and oral mucosa in response to the action of certain chemicals on the body, including drugs. The so-called lichenoid reactions have been described in people whose work is related to the development of color film, who have contact with paraffinylenediamine, who have taken tetracycline (tetracycline lichen), para-aminosalicylic acid (PAS), gold preparations, etc. Thus, the disease in some cases may present is an allergic reaction to certain medicinal and chemical irritants.
Clinical manifestations of LP are characterized by the formation of a monomorphic rash, consisting of flat, polygonal, with a shiny surface and centrally recessed papules of pinkish-violet or crimson-reddish color, with a diameter of 2–3 mm. On the surface of the papules there is a peculiar shine with a waxy tint, which is especially noticeable in side lighting. Papules, merging, form small plaques, on the surface of which there are small scales. When the surface of papules and especially plaques is lubricated with vegetable oil, small whitish dots and intertwined web-like stripes appear through the stratum corneum (Wickham's symptom), this is due to uneven thickening of the granular layer of the epidermis. When pathological lesions resolve, persistent hyperpigmentation often remains. Dermatosis is accompanied by itching, often very intense, depriving patients of rest and sleep [1, 7–10, 15, 19].
LLP is localized on the flexor surfaces of the forearms, in the area of the wrist joints, on the inner surface of the thighs and extensor surfaces of the legs, as well as in the inguinal and axillary areas, and the oral mucosa. The pathological process usually does not involve the skin of the face, scalp, palms and soles. In the area of the extremities, the rash may have a linear (zoniform) arrangement.
About 25% of patients with LP have only lesions of the mucous membranes (mouth, glans penis, vestibule of the vagina) and are not accompanied by manifestations on the skin. On the mucous membrane of the cheeks, grayish-opaline dotted papules are formed, grouped in the form of rings, networks, laces, on the surface of the tongue - flat, whitish opal plaques with clear jagged edges, reminiscent of foci of leukoplakia, on the red border of the lips (usually the lower) - small purple ones plaques, slightly flaky, with a grayish-white mesh on the surface [1, 7–10, 15, 19].
Changes in nails with pronounced longitudinal striations, sometimes in the form of ridges, hyperemia of the nail bed with focal clouding of the nail plates of the hands and feet are observed in some patients with LP [1, 15].
LCP is characterized by an isomorphic reaction to irritation. Often, typical elements of dermatosis are located linearly at the sites of excoriation (Koebner phenomenon). The disease lasts a long time, often for many months. There have been cases of generalization of dermatosis with the development of secondary erythroderma (lichen ruber planus generalisata) [1, 7–10].
Several atypical forms of lichen planus are identified [2, 3, 17]:
- hypertrophic, warty form (lichen planus hypertrophicus, seu verrucosus);
- atrophic and sclerotic forms (lichen planus atrophicus, lichen planus sclerosus);
- pemphigoid, or vesicular, form (lichen ruber pemphi goides, seu bullosus);
- lichen ruber moniliformis (lichen ruber moniliformis);
- pointed, perifollicular form (lichen planus acuminatus, sen planopilaris);
- erosive-ulcerative form (mucous membrane).
Diagnosis . With classic manifestations of LP, diagnosis is not difficult and it is established clinically. In doubtful cases, histological examination can help, where a typical mononuclear infiltrate will be present, disrupting the basal line of keratinocytes [1, 3].
In some patients, differential diagnosis of LP with psoriasis and syphilis is carried out, since lichen planus rashes on the skin may resemble psoriatic elements and syphilitic papules. However, papules in LLP have the characteristic color of the rash, a polygonal shape, an umbilical depression in the center of the papules, a Wickham grid, and the absence of the phenomena of stearin stain, varnish film and pinpoint bleeding allows us to differentiate lichen planus with psoriasis. Papules are round and hemispherical in shape, their “ham” color, density, positive serological reactions to syphilis make it possible to distinguish syphilitic papules. It may be difficult to make a diagnosis if the rash is localized on the oral mucosa.
The clinical picture of LP of the oral mucosa is differentiated from leukoplakia, lupus erythematosus, syphilitic papules and other diseases.
Leukoplakia, unlike LP, has keratinization in the form of a solid grayish-white plaque and does not have a patterned lesion.
In lupus erythematosus, the lesion is hyperemic, infiltrated, hyperkeratosis is present only within the focus of inflammation in the form of tender points, short stripes, sometimes merging along the edge of the lesion in the form of stripes and arcs; in the center of the lesion there is atrophy, which will not occur with LP.
Syphilis papules are usually larger, round or oval in shape, their surface is covered with a grayish-white coating, which is usually removed when injured, and pale treponemas are found on their surface. Positive serological reactions to syphilis [1, 3, 15, 19].
Treatment approaches
LLP is often a chronic but benign disease, sometimes asymptomatic, and does not require systemic treatment. However, taking into account the frequent chronicity of the process and the many severe and atypical forms, the complexity of its pathogenesis, successful treatment is possible only with complex and individualized treatment using modern tools and methods [4, 11, 16, 18].
It is especially important to consider the factors that contributed to the onset of the disease. It is necessary to eliminate risk factors - household and professional hazards, concomitant diseases, foci of focal infection. They carry out sanitation of the oral cavity and prosthetics. Food products should not cause irritation to the mucous membranes of the mouth. Attention is paid to previous treatment and drug tolerance [11].
Due to the fact that the material basis of the disease is immune inflammation (delayed-type hypersensitivity reaction - DTH), correction of immunity is of particular importance and the disease itself responds well to immunosuppressants. To interrupt the cooperative connection of immunocompetent cells, glucocorticosteroids in combination with 4-aminoquinoline derivatives (hydroxychloroquine, chloroquine) are prescribed as basic therapy, especially for common and resistant forms. However, drugs that suppress immune processes should be used only in the presence of documented visceral damage or if the erosive process interferes with eating or speaking.
In the presence of intense itching, in the acute period of the disease, histamine H1 blockers and antiserotonin drugs and catecholamine blockers are indicated. Along with this, sedatives and antidepressants are prescribed to help normalize sleep and reduce itching.
Vitamin therapy has a beneficial effect on metabolic processes. The proliferation and differentiation of keratinocytes is influenced by vitamin A (daily dose for adults - 100,000 IU). Retinoids - derivatives of vitamin A (Tigazon, Neotigazon, Etretinate) reduce the intensity of the inflammatory reaction, affect the condition of cell membranes and normalize proliferation processes. Retinoids are effective against lesions of the oral mucosa and red border of the lips. In recent years, analogues of vitamin A - carotenoids - have been successfully used, especially in atypical forms, in particular erosive-ulcerative, as well as in cases of damage to the oral mucosa and genital organs.
Vitamin E (alpha-tocopherol acetate), used as an antioxidant and inhibitor of the cytochrome P450 system, allows for complex treatment with corticosteroids to reduce the daily dose and shorten the duration of steroid therapy. The multivitamin preparation Aevit is indicated for patients with a long-term chronic course of the disease, with verrucous forms and damage to the mucous membranes.
In chronic relapsing dermatosis, agents that improve oxygen supply to tissues are indicated.
External treatment with applications of corticosteroid ointments, solutions and shaken mixtures with menthol, anesthesin, citric acid, and antihistamines is prescribed for intense itching. Hypertrophic foci are destroyed by cryodestruction or electrocoagulation. Erosive-ulcerative lesions are subject to local treatment with epithelizing agents, including Solcoseryl, sea buckthorn oil, and rosehip oil.
Currently, the method of combined phototherapy (UVAB, ultraviolet irradiation) is successfully used. This therapy affects immune responses by damaging immune cells in the skin. At the same time, the superficial lymphocytic infiltrate in the dermis disappears, and the cellular composition in the epidermis is normalized.
Of the listed means and methods, only their rational choice - sequential stage-by-stage (course) application, taking into account the individual characteristics of the patient and the nature of the course of the disease - allows one to achieve positive results.
Recently, immunotropic therapy for lichen planus has been increasingly used, including the use of exogenous interferons (Reaferon, Interlock) and interferonogens (Neovir, Ridostin).
If the disease is suspected to be caused by any drug or chemical, its use should be discontinued. A thorough examination of patients is necessary to identify internal diseases. First of all, you need to examine the gastrointestinal tract, blood sugar levels, and neuropsychic state [1, 11, 15, 19].
In the absence of symptoms, treatment is not required. To reduce itching, antiallergic drugs are used. The doctor may also prescribe vitamins, sedatives, and physiotherapy.
Physiotherapeutic procedures include electrosleep, diadynamic paravertebral currents, and inductothermy of the lumbar region. Antipruritic shaken suspensions, corticosteroid ointments, 2–5% tar-naphthalan ointments are prescribed externally. The prognosis for life is favorable.
As with any chronic process, LP requires local and systemic therapy [15, 19].
Local drugs of choice are corticosteroids. Class I and II corticosteroids are prescribed. For verrucous process, occlusive dressings with class II corticosteroids are recommended. Intralesional administration of drugs is used, but this method should only be used for very persistent verrucous plaques.
Corticosteroids are effective for lichen planopilaris of the scalp, but they should be applied to the periphery of the plaque and not to its center. Also, betamethasone preparations in the form of foam are very suitable for this localization of the lesion.
For mucosal lesions, especially if they are erosive or ulcerated, triamcinolone pastes or gels are prescribed, which improves the condition in 65% of such patients after 2 weeks. The use of 0.025% fluocinolone based on 4% hydroxycellulose gel in combination with chlorhexidine and miconazole gel for an antifungal effect improved the condition in 50% of patients and served as a prevention of oral candidiasis.
You can rinse the mouth for 5 minutes with one soluble tablet (500 mcg) of betamethasone, originally intended for systemic use. However, this rinsing method is only useful for lesions that have eroded de novo and not for lesions that have eroded due to trauma.
Fluocinonide 0.025% 6 times a day for 2 months is active compared to placebo and without side effects. Betamethasone valerate in aerosol form was used for 2 months with good results in 8 of 11 patients. Clobetasol propionate 0.05% was recently found to be more effective than fluocinonide 0.05%.
Intralesional administration of corticosteroids has been used for lichen planus of the oral mucosa. The preferred drug is triamcinolone acetonide, which is prescribed at a dose of 5–10 mg/ml weekly or twice a week for 3–4 weeks [4, 18, 19].
Topical retinoids are used for lesions in the oral cavity. Fenretinide, for example, gave excellent results when used twice daily, with no local or long-term side effects. Retinoic acid 0.1%, tretinoin 0.025%, and isotretinoin gel 1% were all effective, but less effective than topical triamcinolone or flucinonide [19].
Systemic treatment
Cyclosporine A (CyA) specifically targets cell-mediated hypersensitivity reactions and is the drug of choice for LP. The initial dose is usually 5 mg/kg/day. It is reduced to 2 mg/kg/day as soon as possible: regimens with a treatment duration of more than 6 months should be avoided. Blood pressure should be monitored weekly and kidney function monthly. The best indication for the use of CyA is severe erosive LP.
Systemic corticosteroids may be used instead of CyA. Prednisone can be prescribed at a dose of 1 mg/kg/day (or a lower dose). The dose is reduced over 1 month. When the drug is discontinued, a rebound effect may occur. Common side effects of corticosteroids are common.
For erosive LP with chronic active hepatitis, azathioprine (50–100 mg/day) is recommended. Normalization of transaminase levels is usually accompanied by improvement of lesions in the oral cavity. However, if a patient has antibodies to the hepatitis C virus, all immunosuppressive treatments should be avoided, since immunosuppressive drugs may contribute to the development of liver cancer.
Other drugs that have been shown to be beneficial in reversing the clinical process of LP include thalidomide, hydroxychloroquine, retinoids, and levamisole.
Hydroxychloroquine is used at a dose of 200–400 mg/day for several months in patients who have lesions in the oral cavity. When analyzing the risk-benefit ratio, retinal side effects must be taken into account and carefully monitored.
For systemic treatment of LP, acitretin (0.25–0.75 mg/kg/day) and isotretinoin (0.25–0.50 mg/kg/day) are used. However, these drugs should not be prescribed to women of childbearing age due to their well-known teratogenicity [19].
In severe forms of erosive oral lichen planus that do not respond to traditional treatment, PUVA therapy (PUVA = Psoralens + UltraViolet A) can have a positive effect. A dose of 0.6 mg/kg 8-methoxypsoralen is administered orally 2 hours before irradiation with long-wave ultraviolet light. In one study, irradiation was administered 12 times at 2–3 day intervals for a total dose of 16.5 J/cm2. In another study, 20 sessions were performed, 3 per week, with a total cumulative dose of 35.9 J/cm2. After treatment, clinical symptoms and erosive lesions disappeared. Side effects are similar to those observed after whole body PUVA therapy [16, 19].
Evaluation of treatment effectiveness. Provided that the therapy is correctly selected, regression of the pathological process occurs within 1–2 weeks, the rash disappears after 1–1.5 months. Clinical cure (recovery) is characterized by the complete disappearance of papules, in the place of which hyperpigmented or depigmented spots remain. The latter can remain for an indefinite period of time (from several weeks to several months). Erosive-ulcerative, hypertrophic and atrophic forms of lichen planus are usually resistant to therapy, and the rashes persist for several months or even years.
Primary prevention consists of sanitation of foci of chronic infection, treatment of psychoneurological disorders; Overwork and stress should also be avoided. Prevention of exacerbations: prescribing water treatments - baths, showers (not recommended in the acute period of the disease), hydrogen sulfide and radon baths; diet (exclusion from the diet of coffee, spices, chocolate, honey, alcohol) [1, 10, 17, 19].
Literature
- Bazyka D. A., Bazyka A. D. Etiology, pathogenesis and therapy of lichen planus // Vestn. derm. and veins 1977, No. 11, p. 58.
- Gadzhimuradov M.N., Gunaeva A.A. Atypical forms of lichen planus: clinical manifestations, differential diagnosis and treatment // Clinical dermatology and venereology. 2009, No. 3, p. 85–80.
- Differential diagnosis of skin diseases. Ed. B. A. Berenbein and A. A. Studnitsyn. M., 1983. P. 269.
- Korsunskaya I.M., Nevozinskaya Z.I., Zakharova A.B., Konstantinov E.M., Andryushkova Yu.A. Experience in the treatment of lichen planus with the drug Glutoxim // Russian Journal of Skin and Venereal Diseases. 2008, No. 1, p. 44–46.
- Maksimovskaya A. N., Tsarev V. N., Guseinova S. S. Bacteriological basis for the treatment of lichen planus of the oral mucosa using laser radiation. In the book: Proceedings of the VI Congress of the Russian Dental Association. M., 2000, p. 275–277.
- Manukhina O. N. Clinical course of lichen planus of the oral mucosa against the background of decreased functional activity of the thyroid gland. M.: Science to Practice, 1998. pp. 145–147.
- Mashkilleyson A. L. Diseases of the mucous membrane of the oral cavity and lips. M.: Medicine 1963. P. 188.
- Pashkov B. M. Lesions of the oral mucosa in skin and venereal diseases. M.: Medicine 1963. P. 182.
- Petrova L.V. Features of the clinical course of lichen planus of the oral mucosa // Ros. magazine cutaneous veins bol. 2002; 3:28–31.
- Pototsky I.I. Directory of dermatovenerologist. Kyiv, 1985. P. 88.
- Rabinovich O. F. Immunological aspects of the pathogenesis of lichen planus of the oral mucosa (clinic, diagnosis, treatment). Diss. Dr. med. Sci. M., 2001, 190 p.
- Raikhlin A. N. Subcellular mechanisms of development of lichen planus of the oral mucosa and its treatment: Abstract of thesis. dis. ...cand. honey. Sci. M., 1986.
- Slesarenko N. A. Lichen planus (modern immunological and biochemical aspects) and methods of pathogenetic therapy: Abstract of thesis. dis. ...Dr. med. Sci. M., 1995.
- Spitsyna V.I. Pathogenesis of immunodeficiency in patients with lichen planus of the oral mucosa // Russian Dental Journal. 2002, No. 3, p. 30–34.
- Thomas P. Habiff. Skin diseases. Diagnosis and treatment. M.: “MEDpress-inform”, 2008. 672 p.: ill.
- Faizulin R. A. The use of dimocyphon and selective phototherapy of patients with lichen planus, taking into account immunological blood parameters: Abstract of thesis. dis. ...cand. honey. Sci. M., 1992. 21 p.
- Fedorov S. M., Selissky G. D., Timoshin G. G. Lichen planus // Skin diseases. M.: GEOTAR-Medicine, 1997. pp. 67–69.
- Khamaganova I.V. Advantan (methylprednisolone aceponate) in the complex treatment of lichen planus // Bulletin of Dermatology and Venereology. 2004, No. 3.
- Rebora A. Lichen planus. European guidelines for the treatment of dermatological diseases. Ed. A. D. Katsambasa, T. M. Lotti. M.: “MEDpress-inform”, 2008. pp. 371–374.
A. S. Bisharova, Candidate of Medical Sciences
GBOU DPO RMAPO Ministry of Health and Social Development of Russia, Moscow
Contact information about the author for correspondence
Symptoms of the disease
There are six types of oral lichen planus. This is a typical, exudative-hyperemic, hyperkeratotic, erosive-ulcerative, bullous and atypical form. They are united by the formation of foci of inflammation on the oral mucosa, the appearance of defects and erosions. In some particularly severe forms of the disease, the patient may complain of itching and burning sensation in the mouth and difficulty eating. In milder forms, the disease may not manifest itself at all.
Typical lichen planus is the most common form, occurring in half of patients. White nodules appear on the mucous membrane of the oral cavity. Merging, they resemble lace.
The esscudative-hyperemic form is characterized by the appearance of gray papillomas on the edematous mucous membrane.
The hyperkeratotic form is one of the least common forms, which is characterized by the formation of gray spots that rise above the affected surface. Over time, these plaque spots become rougher and flake off.
Erosive-ulcerative is the most severe form of the disease, occurring in 23% of cases. Multiple erosions and ulcers covered with fibrinous plaque appear on the lining of the oral cavity. There is a strong burning sensation in the mouth, and when trying to remove plaque, bleeding and pain occur.
The bullous form is a relatively rare variety, occurring in 3% of cases. Accompanied by the appearance of dense blisters, inside of which there is hemorrhagic exudate. After the bubbles open, erosions form.
Atypical form - occurs slightly more often than bullous - in 4% of cases. This form is characterized by dilation of the mouth of the salivary gland, as well as inflammation of the lips and gums.
Quite often, one patient can develop several forms of lichen planus in parallel. Often one form can flow into another. Ringworm is a chronic disease prone to relapse.
Material and methods
The study was carried out with the participation of 147 patients with various forms of LP of the oral mucosa, aged from 24 to 70 years, who sought advice from dental clinics at the Ural State Medical University and the Bashkir State Medical University.
The examination of patients with LP of the oral cavity included a thorough collection of anamnesis of this disease, clarification of hereditary predisposition taking into account previous diseases, identification of comorbid conditions and their relationship with the main one, the stages of manifestation of clinical symptoms of LP (periods of exacerbation and remission), allergic factor, and, if necessary, cytological and histological research.
When examining the mucous membranes, tongue and lips, attention was paid to the presence of signs of inflammation, elements of damage, and their location. An important diagnostic value is the presence of an isomorphic reaction in LP (Koebner's symptom), manifested by the appearance of fresh primary elements characteristic of this disease at the site of irritation of the skin or mucous membrane by any exogenous factor.
Treatment
For different forms of the disease, a different course of medications is prescribed. If the disease is asymptomatic, drug treatment may not be necessary. If erosions and ulcers have already formed, it is necessary to begin treatment as quickly as possible to avoid worsening the condition.
Inflammatory processes are controlled by the use of corticosteroids. Local treatment is carried out to relieve pain and accelerate tissue regeneration. To avoid the development of candidiasis, antifungal drugs are prescribed.
Electrophoresis and phonophoresis are also effective. In rare cases, when erosions do not heal for a long time, surgical intervention is indicated.
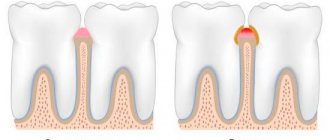
In all cases, without exception, the oral cavity is sanitized and the source of inflammation is removed (for example, periodontitis, caries or pulpitis).