Pathological changes in the oral cavity, as well as diseases of the oral mucosa are one of the symptoms of the presence of the immunodeficiency virus in the body. However, one should not think that the presence of dental problems may indicate infection with the immunodeficiency virus. To understand how oral diseases are related to HIV infection, it is worth talking in more detail about the immunodeficiency virus and its vital functions.
What is HIV? What is HIV infection
The human immunodeficiency virus, or HIV, was identified and described relatively recently. Invading the human body, it primarily affects macrophage cells and T-lymphocytes, which are responsible for recognizing and destroying hostile bacteria. Thus, the body's immune barrier loses its ability to resist both external bacterial attacks and internal opportunistic flora.
The immunodeficiency virus is transmitted exclusively through sexual contact or through direct contact of a healthy body with infected blood. Transmission of the virus through household or food contact is impossible.
HIV infection is a slow-onset disease caused by a virus and occurs against a background of suppressed immunity. It can take years from the introduction of the virus to the clinical manifestations of the disease. During this entire period, the virus does not manifest itself in any way, and its presence can only be diagnosed using a laboratory method.
HIV infection of the oral cavity and its causes
Inflammatory processes in the mucous tissues of the oral cavity are one of the first symptoms of virus activation. This is due to the peculiarity of the structure of the oral cavity and its constant contact with the aggressive external environment. Most often, the mucous membrane is affected by the herpes simplex virus, Candida fungus, Epstein-Barr virus, and papillomaviruses. Bacterial infections are caused by streptococci and staphylococci, which are no longer contained by local immunity. In conditions of immunity suppressed by the virus, periods of remission become shorter, and inflammatory processes are acutely progressive. Timely prescribed additional studies make it possible to correctly prescribe a course of maintenance therapy, since diseases of the oral mucosa are not directly a symptom of HIV infection.
Based on their suspected association with HIV, oral infections are divided into three groups.
Group 1 includes pathologies most closely associated with the immunodeficiency virus:
- candidiasis, colloquially “thrush”;
- hairy leukoplakia (changes in the mucous membrane of the tongue);
- HIV gingivitis (acute inflammation of the gums);
- HIV periodontitis (periodontal inflammation);
- Kaposi's sarcoma (a specific neoplasm on the hard palate of the oral cavity);
- non-Hodgkin's lymphoma.
The 2nd group of diseases includes lesions to a lesser extent, associated with symptoms of HIV infection:
- thrombocytopenic purpura (multiple hemorrhages);
- pathology of the salivary glands;
- viral infections (herpes).
Group 3 includes diseases that often occur with HIV infection, but are not associated with it. Below we will consider diseases from the first group, as the most characteristic of the state of immunodeficiency.
Specifics of treatment of dental diseases
The success of treating oral lesions and dental diseases associated with HIV depends on making a timely and correct diagnosis. Therapeutic methods are more effective against the background of highly active antiretroviral therapy.
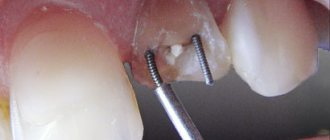
As a rule, specialists select medications with minimal side effects, and surgical interventions, for example, a tooth extraction , are carried out under the control of blood clotting. In this case, treatment should be as atraumatic as possible.
In addition, strict oral hygiene is recommended for HIV-infected people.
It is important for doctors to remember about prevention when examining the oral cavity of patients infected with HIV. The main danger is contact with the patient’s infected blood on the skin, mucous membranes of the eyes, mouth, and nose. When examining and manipulating the oral cavity of patients with HIV and AIDS, specialists are recommended to use double latex gloves, a protective screen, wear protective clothing made of non-woven material and observe other precautions.
List of sources
1. HIV infection in adults. Clinical recommendations. National Association of Specialists in the Prevention, Diagnosis and Treatment of HIV Infection // Ministry of Health of the Russian Federation. 2022. // URL: https://rushiv.ru/wp-content/uploads/2019/03/kr79.pdf (access date: 06/13/2020).
2. HIV/AIDS // WHO Information Bulletin. July 25, 2022 // URL: https://www.who.int/ru/news-room/fact-sheets/detail/hiv-aids (access date: 06/13/2020).
3. Help. HIV infection in the Russian Federation as of April 30, 2020 // Federal Scientific and Methodological Center for the Prevention and Control of AIDS of the Central Research Institute of Epidemiology of Rospotrebnadzor. // URL: https://www.hivrussia.info/wp-content/uploads/2020/05/VICH-infektsiya-v-Rossijskoj-Federatsii-na-30.04.2020-g..pdf (date of access: 13.06. 2020).
4. Polyanskaya L.N. Features of manifestations of HIV infection in the oral cavity // Modern dentistry. 2022. No. 1 (66). // URL: https://cyberleninka.ru/article/n/osobennosti-proyavleniy-vich-infektsii-v-polosti-rta (date of access: 06.13.2020).
5. Petrov A. A. Providing dental care to HIV-infected patients // Bulletin of SMUS74. 2016. No. 4 (15). // URL: https://cyberleninka.ru/article/n/okazanie-stomatologicheskoy-pomoschi-vich-infitsirovannym-bolnym (date of access: 06/07/2020).
Symptoms of HIV infection in the oral cavity
The herpes simplex virus is present in most people. The infection persists in the body throughout life and does not cause any special problems, except for rare rashes on the lips.
Herpetic gingivostomatitis
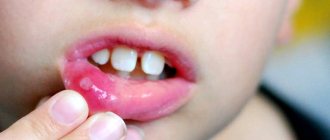
In HIV-infected people, herpes rashes are chronic with rare stages of remission. It is distinguished by blistering rashes around the mouth and on mucous tissues. When the vesicles open, painful erosions occur that develop into fairly large ulcers. The manifestation of herpes zoster and rashes in atypical places is also noticed.
Candidiasis
Candidiasis is also a common symptom of HIV infection and is chronic. Its symptoms are the same as with regular thrush, the only difference being that plaque covers most of the mouth.
Hairy leukoplakia
Clinical manifestations of the disease look like deformed mucous tissue, externally resembling folds or hairs. Localization area: lateral parts of the tongue and the inner surface of the cheeks. Painful sensations are usually absent.
HIV gingivitis and periodontitis
In this case, the infection manifests itself as acute inflammation of the gums. Starting with ordinary bleeding gums, the disease quickly develops into an acute form. With adequate treatment, tooth loss can be avoided.
Kaposi's sarcoma
This is one of the most characteristic symptoms of HIV infection in the clinical stage of manifestation. The tumor is formed from lymphatic vessels, in the mouth it is located near the root of the tongue, less often on the gums.
Candidiasis
Cervical cancer
Diabetes
HIV
Thrush
19300 July 27
IMPORTANT!
The information in this section cannot be used for self-diagnosis and self-treatment.
In case of pain or other exacerbation of the disease, diagnostic tests should be prescribed only by the attending physician. To make a diagnosis and properly prescribe treatment, you should contact your doctor. Candidiasis: causes, symptoms, diagnosis and treatment methods.
Candidiasis is an infectious disease caused by yeast-like fungi of the genus Candida. It is caused by the active proliferation of fungus on the mucous membranes of the oral cavity, genital and internal organs and on the skin.
All representatives of the genus Candida belong to opportunistic microorganisms, that is, they are constantly present in the normal microflora. But with a decrease in immunity, changes in hormonal levels and for a number of other reasons, these fungi can begin to actively colonize the mucous membranes and skin.
The most common members of the genus are Candida albicans and C. tropicalis. In 90-95% of cases of urogenital candidiasis, C. albicans is the dominant pathogen.
The first contact with fungi of the genus Candida occurs during the passage of the child through the birth canal. However, the medical literature describes cases of detection of these microorganisms in amniotic fluid, which indicates the possibility of a vertical (transplacental) transmission route. Transmission of the fungus of the genus Candida also occurs through breastfeeding, skin contact between the child and the mother, and through household and food routes.
These microorganisms produce endotoxins and enzymes that cause cell death and tissue necrosis, which enhances the adhesive (attachment to cells of the mucous membranes or skin) ability of the fungus and ensures penetration into tissue.
Overproduction of these and a number of other substances determines the pathogenicity of representatives of the Candida family.
Causes of candidiasis
- Exogenous (external) factors facilitating the penetration of fungi into the body:
- occupational hazards leading to frequent skin damage;
- prolonged exposure to a warm and humid environment;
- violation of the integrity of the mucous membranes.
- Factors leading to a decrease in the body's resistance:
- presence of chronic diseases;
- long-term use of drugs that disrupt the natural microflora;
- unbalanced diet;
- frequent stress, disturbances in sleep and rest patterns.
Risk factors for developing candidiasis
- Metabolic disorders (hypovitaminosis), diseases of the immune system (HIV infection), endocrine pathologies (diabetes mellitus, etc.).
- Long-term use of certain drugs: hormonal contraceptives, systemic glucocorticosteroids, broad-spectrum antibiotics, cytostatics.
- Long stay or living in an area with high humidity and temperature, comfortable for the circulation of fungal spores in the environment.
Classification of the disease
Based on the localization of the process, the following are distinguished:
- Urogenital candidiasis.
- Candidiasis of the oral mucosa.
- Superficial candidiasis.
- Interdigital candidiasis.
- Candidiasis of periungual ridges and nails.
- Candidiasis of the gastrointestinal tract.
Symptoms of candidiasis
Urogenital candidiasis (UGC)
– a widespread disease: according to medical statistics, about 75% of women of reproductive age have registered symptoms of UGC at least once.
There are acute and chronic forms of urogenital candidiasis, candidiasis of the vulva, vagina and other urogenital localizations.
In some cases, when diagnosing, a clarification is used: complicated or uncomplicated UGC, which reflects the number of exacerbations per year and the severity of the disease. Symptoms of female urogenital candidiasis
- The appearance of white-yellow cheesy or creamy discharge from the genital tract. The intensity of discharge may increase before menstruation, which is associated with changes in hormonal levels.
- Unpleasant sensations, itching in the genital area, often aggravated by sexual intercourse or urination.
- Redness and swelling of the mucous membrane of the vulva and vagina, the presence of damage to the skin of the genital organs (cracks, microtraumas).
- In the chronic course of UGC, dryness of the mucous membranes of the genital tract develops.
Symptoms of male urogenital candidiasis
- Redness, swelling, discomfort in the genital area.
- Whitish discharge of a cheesy structure from the genital tract.
- Pain and burning during sexual intercourse and urination.
Superficial candidiasis
can be erythematous (the main symptom is reddened areas of the skin with a weeping surface) and vesicular (the formation of papules, vesicles and pustules in the affected area - inflammatory elements located in the superficial layers of the skin). The lesion begins with large folds of skin, gradually spreading to other areas of the body. In the depths of the folds, weeping occurs (separation of serous exudate through the smallest defects of the epidermis), a violation of the integrity of the skin contributes to the addition of a secondary infection.
Interdigital candidiasis
localized in the space between the fingers. In this case, redness of the skin is noted, followed by the appearance of bubbles in transparent contents. The disease spreads quickly in close groups (in kindergartens, schools, etc.).
Oral mucosal candidiasis (OCOR)
Oral candidiasis causes discomfort, especially when eating - burning, pain, dryness. Depending on the location of the process, several forms of oral candidiasis are distinguished.
Often, CSOPR and the gastrointestinal tract accompanies immunodeficiency conditions: HIV infection, acquired human immunodeficiency syndrome (AIDS) or congenital immunodeficiency (for example, with T-lymphocyte pathology). In the presence of these diseases, candidiasis occurs with the most severe symptoms, is difficult to treat, and is aggressive in nature.
The most common manifestation of CSOPR is candidal stomatitis, which mainly affects infants and adults with weakened immune systems.
With this pathology, the oral mucosa turns red, swells, and whitish films with a cheesy consistency appear on it. In the initial stages of the disease, plaque is easily removed. As the disease progresses, the films become denser, are difficult to separate, and when removed, the bleeding mucous membrane is exposed.
With candidal stomatitis, the tongue may be affected, which is manifested by redness of the back of the tongue, the appearance of plaque and desquamation of the epithelium. These symptoms are accompanied by severe pain in the affected area when talking, eating, and palpating the tongue.
Smokers, more often than other types of CSOPR, develop chronic hyperplastic candidiasis, accompanied by the formation of white, merging plaques that rise above the surface of the hyperemic mucosa.
With this pathology, the consistency of saliva changes: it becomes viscous and foaming; there is an unpleasant odor from the mouth, a gray or white coating on the mucous membrane. In 10-40% of cases, this clinical form of candidiasis becomes malignant (i.e., becomes malignant).
Older people most often develop a chronic atrophic form of oral candidiasis. The mucous membrane turns red and swells. The lesion is often localized under dentures, which causes pain.
Candidal cheilitis and candidiasis of the corners of the mouth mainly occur in children and the elderly. The lesion is usually bilateral, with the formation of red, painful cracks in the corners of the mouth, covered with an easily removable white coating or scales. With a long course of the disease, a bacterial infection may occur.
Diagnosis of candidiasis
The diagnostic search algorithm for candidiasis of any localization includes taking material from the affected area, followed by microscopy and culture to determine the type of fungus and its sensitivity to antimycotic (antifungal) drugs.
In order to diagnose conditions that lead to a decrease in immunity, a general blood test is used;
Diagnosis for suspected HIV infection
For differentiated diagnosis of HIV infection from similar dental diseases, the following tests are used:
- Blood test for PCR reaction (aimed at detecting HIV).
- Immunoblotting technique.
- Linked immunosorbent assay.
- Checking immune status.
If the results are unclear, additional blood tests, as well as bacteriological studies, may be prescribed. Early diagnosis of the root cause of diseases can significantly alleviate the course of the disease.
Diagnosis of human immunodeficiency virus
It is important for any person to know what HIV tests are available in clinics. To detect infection, an enzyme-linked immunosorbent assay is performed to detect antibodies to HIV in biological fluids. A positive result can only be after the end of the incubation period, when the body has already synthesized antibodies to the virus. The test is done no earlier than 4 weeks after contact, the results will be reliable after 3-4 months, control tests are taken after 6 and 12 months.
If the ELISA is positive, the blood sample is retested by immunoblotting. If this test gives a positive answer, the probability of HIV reaches 99.9%. If the immunoblot test is negative, there is no virus in the blood. An indeterminate test result is possible during the incubation period, when there are still few viral particles, or after treatment of the infection.
If HIV is detected, the patient is given tests to measure the amount of viruses in the blood plasma (the so-called viral load) and the patient's immune status is determined.