What is this disease?
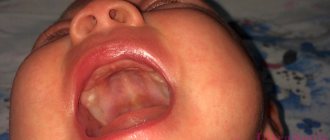
Herpetic stomatitis is a pathological process that develops in the mucous membrane lining the oral cavity. The causative agent of this disease is herpes simplex virus type 1. In children under the age of five, this virus is detected in 60% of all cases. By adolescence, it is detected in the vast majority of people. Herpes stomatitis in children develops during the baby’s first contact with the virus. This occurs most often before the age of three.
The high incidence is explained by:
- low level of production of own antibodies;
- immaturity of cellular immunity;
- the fact that the baby does not receive antibodies from mother's milk;
- high reactivity of the child's body.
If the baby is bottle-fed, he may get sick in the first months of life. Viral infection often goes into a latent state. It persists in the nerve ganglia.
Causes of stomatitis
Inflammation of the oral mucosa can be caused by various reasons.
- Mucosal injury6.
- Viral, bacterial or fungal infection6.
- Allergy2.
- Immunity disorders (autoallergy, that is, a reaction to one’s own altered tissues2).
- Diseases of the blood, digestive, cardiovascular, nervous and endocrine systems2.
- Hypovitaminosis - lack of vitamins C, B1, B12, E, D32.
- Common infectious processes: measles, rubella, scarlet fever and diphtheria, infectious mononucleosis, tuberculosis and others1.
Only a specialist can understand the causes of stomatitis. Therefore, if symptoms of the disease appear, you should definitely contact your dentist.
Inflammatory diseases of the oral cavity can occur in a child of any age6. Immaturity of the body is the primary factor predisposing to the occurrence of stomatitis in children under one year of age. The mucous membrane of the oral cavity during this period of a child’s life is very vulnerable, its natural protective properties are reduced. The immunity received from the mother during fetal development and which protected the baby immediately after birth weakens every day. Therefore, the infection easily penetrates the mucous membrane and causes its inflammation. Most often at this age, candidal stomatitis occurs, commonly called thrush1,6.
From the age of one to 3 years, children actively develop immune mechanisms to protect the oral mucosa (local immunity), but its permeability to viruses remains extremely high. Therefore, in a 2-3 year old child, stomatitis is more likely to be viral, in the vast majority of cases - herpetic1,3,4.
From 4 to 12 years of age, stomatitis in children is more often caused by allergic and autoimmune reactions. In particular, chronic aphthous forms of the disease occur during this period1.
Up to contents
Causes
The cause of the development of the pathology is the herpes simplex virus type 1. It belongs to DNA viruses belonging to the Herpesviridae viral family. The pathogen multiplies rapidly in the epithelial cells of the oral mucosa. Then it enters nearby lymph nodes (submandibular) and continues to reproduce in them. Then it enters the blood and migrates to the parenchymal organs (spleen, liver, kidneys). There it multiplies and enters the bloodstream again. As a result, it again appears in large quantities in the epithelial cells of the skin and mucous membranes. They are massively defeated. It is localized in the oropharynx, oral cavity, nose, lips, and nearby skin. Stomatitis and herpes of the skin and mucous membranes develop when the infection generalizes simultaneously.
Children become infected with it as follows:
- through contact and everyday life (using shared utensils, toys, through kissing);
- airborne (coughing, sneezing);
- from a sick mother to the fetus through the placenta or during childbirth.
A baby can become infected from sick adults, children, and carriers.
The following factors contribute to the development of the disease:
- previously suffered inflammatory processes;
- previous antibiotic therapy;
- deficiency of microelements and vitamins in the body;
- mechanical damage to the skin and mucous membranes;
- insufficient fluid intake;
- poor oral hygiene.
In children, the virus is especially easily transmitted through contact. The infectious process quickly spreads to healthy areas.
Symptoms
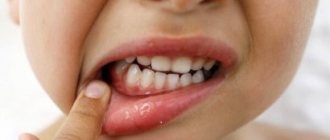
Gingivitis has a main symptom by which it is easily identified - inflammation affecting the child’s gums. The process begins with a slight redness that quickly gains strength. This signal often goes unnoticed by parents, and children go to the dentist with an active inflammatory process, bright red swollen gums, burning, and pain. These signs indicate that the disease has entered an acute phase.
Children suffer most from the catarrhal form of this disease, which can be chronic or acute. In the first case, the symptoms are not pronounced, pain occurs only when brushing, there is slight swelling, redness, and cyanosis of the gums.
A sign of an acute form of the disease is intoxication of the child’s body. It manifests itself as headache, nausea, lethargy, and fever.
The most complex type of disease, ulcerative gingivitis, manifests itself as follows:
- the inflammatory process progresses;
- their structure changes;
- there is an unpleasant odor from the mouth;
- lymph nodes in the neck enlarge;
- saliva is produced profusely;
- the skin turns pale.
If these signs are left unattended, an ulcerative-necrotic form of the disease may occur, when necrotic areas with a gray-green coating and a putrid odor appear on the gums, saliva becomes viscous, body temperature rises and the general condition significantly worsens.. All this indicates severe intoxication in organism.
During puberty in a teenager or if he has problems with hormones, hypertrophic gingivitis occurs. It occurs due to improper orthodontic treatment of dental anomalies. The inflammatory process is accompanied by increased growth of gingival tissue, which leads to partial closure of dental crowns. This form of the disease is usually localized. One or two gums are affected, sometimes the affected area expands. The most common location is the lower anterior incisors and canines.
Atrophic gingivitis does not have a pronounced inflammatory process and occurs without pain, although over time it can be complicated by periodontal disease.
Classification
According to the flow, acute, chronic, and wave-like variants of the pathology are distinguished. The following degrees of severity of the pathological process are distinguished:
- Mild - it is typically characterized by a slight increase in body temperature, moderate inflammation of the mucous membrane in the mouth, and enlargement of regional lymph nodes. Rashes form on the mucous membrane and skin.
- Medium – high temperature rises. Severe weakness and sudden deterioration in health. The baby begins to vomit and the pain in the mouth increases. Significant rashes appear in the mouth and the skin around it.
- Severe - a severe headache is added to the pathological process. High temperature rises, severe muscle pain. Not only regional but also distant lymph nodes enlarge. The rashes are located not only in the oral cavity, but on the skin next to it. They appear on the mucous membrane of the eye, on the eyelids, and on other parts of the face.
The severity of the pathology depends on the viral load (the amount of virus in the body) and the general reactivity of the body.
The essence and causes of thrush
Microscopic yeast-like fungi of the genus Candida live on the mucous membranes and skin of every person. They do not cause harm to health, but only if the immune system suppresses their active reproduction. Otherwise, an inflammatory disease called candidiasis occurs. If fungi colonize the oral mucosa, candidal stomatitis, or thrush, is diagnosed.
The disease is detected in 4-5% of infants. Its main reasons:
- low level of immunity, characteristic of all newborns;
- decrease in protective forces as a result of teething, acute respiratory infections, dysbiosis, intestinal infection, and so on;
- non-compliance with hygiene standards - insufficient cleaning of children's dishes, toys, mother's skin (during breastfeeding);
- antibiotic treatment, which disrupts the balance of bacteria on the mucous membranes;
- drinking sweet tea, water, compote or a mixture - leftover sugar in the mouth contributes to the growth of fungi.
In addition, a baby can “get” too many candida when in contact with adults. Most often, infection occurs during childbirth if the mother has genital thrush. Kissing and sharing utensils can also lead to infection if an adult has candidal stomatitis.
Clinical manifestations
Stomatitis in children is characterized by a gradual onset of the disease. Clinical signs of the disease do not appear immediately after infection. The incubation period is typical for this pathology; it lasts from two days to three weeks.
Symptoms of herpetic stomatitis in children appear starting from the prodromal period.
Each period has its own clinic:
- Latent – lasts up to two weeks. The child's sleep is disturbed and he refuses to eat. The baby becomes restless and whiny. He has increased salivation, possible nausea and vomiting. The lymph nodes are enlarged and painful on palpation.
- The height of the disease - at this time rashes appear on the skin and mucous membranes. They are located on the soft, hard palate, gums, cheeks, lips and tongue. They are group or single, up to three millimeters in size. They are thin-walled bubbles filled with a clear liquid. Their formation lasts up to four days. The vesicles quickly open, then erosions and painful aphthae form. They are shallow ulcers covered with a white coating. The mucous membrane in the mouth is swollen and bleeding. The child develops a high temperature of up to 40 degrees. A runny nose, cough, and conjunctivitis occur.
- Fading - aphthae, erosions gradually heal and epithelialize. These formations heal without scarring. Often there is a wavy course of the disease. The periods of appearance of rashes alternate with rises in temperature.
The illness usually lasts up to two weeks. In children under one year of age, generalization of the process is possible. The development of sepsis, damage to all internal organs and meninges is likely.
White plaque
The tongue and palate of an infant may be covered with a thin whitish coating. Main reasons:
- leftover food;
- mouth breathing;
- thrush.
Leftover food
Immediately after feeding, you can see the remains of breast milk or formula on the baby's tongue and palate. After some time, the plaque disappears on its own. Many pediatricians advise removing traces of food from the baby’s mouth, as they serve as a breeding ground for opportunistic microorganisms.
Cleaning methods:
- give the baby 1-2 teaspoons of boiled water immediately after feeding;
- wipe the epithelial membrane 2 times a day with soda solution or water (the procedure is described below).
If the plaque is easily removed or disappears on its own (it is not present before feeding), do not worry. But in cases where white marks on the tongue, palate and inner surface of the cheeks are constantly present, it is necessary to consult a doctor.
Mouth breathing
If a child breathes through his mouth, his mucous membrane dries out and a whitish coating forms on it. In children under one year of age, this phenomenon is most often caused by acute respiratory viral infections and dry air in the room, which leads to the formation of crusts in the nasal passages.
The only way to prevent the formation of white plaque is to restore nasal breathing in the baby. Basic methods:
- when the mucus dries out, instill saline and oil drops into the nose, as well as humidify the air;
- for a runny nose and congestion due to ARVI - similar measures, in addition, the doctor may recommend the use of vasoconstrictor drops (no longer than 5-7 days).
Diagnostics
A patient suspected of having this disease is examined by a dentist. He asks the child’s parents about how the disease progressed. The diagnosis is established on the basis of the characteristic clinical picture of stomatitis, revealed during examination, anamnesis and characteristic complaints. Upon examination, typical mucosal lesions are revealed.
To confirm the diagnosis, laboratory testing of scrapings of the oral mucosa, the contents of ulcers, the patient’s saliva and blood is used.
The following are used for research:
- cytopolymerase chain reaction;
- immunofluorescence method;
- serological blood tests (RSC, ELISA, immunoglobulin M test);
- HSV test for the detection of immunodot G-specific glycoprotein.
These methods are used only for severe infections, as they are quite expensive.
How to deal with tongue coating
Thorough cleaning of the tongue is the main hygienic measure aimed at eliminating plaque. Clinical trials have shown that regular tongue cleaning reduces bacteria and bad odor by 75%.
How to get rid of dry mouth and white coating on the tongue:
- use a special scraper - effective tongue cleaning reduces plaque by 40%;
- drink enough water;
- eat foods containing coarse fiber (for example, apples, carrots);
- quit smoking;
- do not abuse alcoholic beverages;
- Healthy food;
- rinse your mouth after eating.
By following these simple rules, you can forever “say goodbye” to the coating on your tongue and forget about bad breath.
Related services: Pediatrician consultation
Treatment
Treatment of herpetic stomatitis in children with mild and moderate forms is carried out on an outpatient basis. In severe cases and the development of complications, the baby is hospitalized. Treatment is carried out under the supervision of a pediatric dentist or periodontist.
Children are prescribed bed rest and a diet with pureed, non-irritating food. He is given separate hygiene items and dishes. Plenty of warm fluids are recommended.
The following drugs are prescribed:
- Non-steroidal anti-inflammatory drugs (Nise, Paracetamol, Nurofen) are used to relieve temperature and inflammatory reactions.
- Antihistamines (Clemastine, Loratadine) are used to relieve swelling of the mucous membranes.
- Antiviral drugs (Famciclovir, Acyclovir, Zovirax) are used at the beginning of treatment or in severe cases.
- Immunomodulators (Lysozyme, Gamma globulin, Thymogen) are used to enhance immunity.
During treatment, vitamin-mineral complexes and fish oil are used in monthly courses.
Local drugs that act directly on the mucous membrane are widely used.
For local treatment of herpetic stomatitis the following are used:
- antiseptics (Hexoral, Miramistin) - they are used to rinse the mouth every four hours for two weeks;
- ointments and gels with anesthetics (Kamistad, Lidochlor gel) are used for pain relief, they are lubricated with mucous membranes three times a day for up to two weeks;
- antiviral agents (Ganciclovir, Acicovir) - destroy the viral cell, gums are treated with these ointments five times a day, two weeks;
- proteolytic enzymes (Trepsin, Chymotrypsin) are used to cleanse the necrotic surfaces of ulcers; they are washed with these solutions twice a day.
- rinsing with decoctions of medicinal herbs (calendula, chamomile, sage) is carried out after each meal for up to two weeks;
- epithelializing ointments (Solcoseryl, Methyluracil) are used to enhance the healing of erosions and ulcers, used in the recovery stage, used up to four times a day for ten days.
Physiotherapy is applied locally. Irradiation of affected mucous membranes with ultraviolet and infrared rays is used.
Treatment of white plaque on the palate of a child
The white spots will disappear if the cause of the problem is eliminated. If you regurgitate frequently, for example, you should change your feeding method and sterilize your utensils. A small area of fungal infection is treated with topical preparations. Severe forms of the disease are treated medicinally using complex drugs. Fungal diseases are dealt with:
- Clotrimazole;
- Candide;
- Pimafucin;
- Fluconazole;
- Diflucan;
A sterile gauze ball is moistened with the solution. They gently wipe the oral cavity several times a day. The duration of therapy depends on the complexity of the situation. Treatment usually lasts 7-10 days. Irrigation or lubrication is also prescribed. To boost the body’s defenses, doctors recommend vitamin complexes and probiotics for children. This will restore the natural microflora in the intestines.
Prevention
Preventive measures are aimed at preventing infection. This presents certain difficulties, since the vast majority of the population is infected with it. It is better if the child gets sick from it at an older age.
For this it is recommended:
- avoid contact with infected people;
- will provide personal utensils and personal hygiene products for the child;
- Kissing people with herpetic rashes is prohibited;
- strengthening the baby's immune system.
It is recommended that the child be provided with adequate nutrition and regularly given vitamin and mineral complexes.