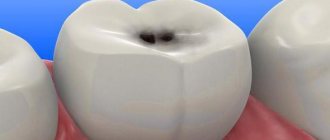
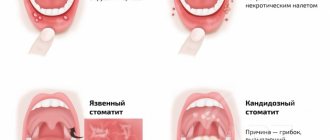
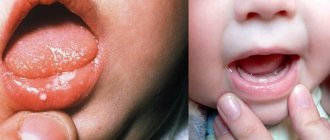
Classification of gingivitis according to intensity
- easy
- average
- heavy
The severity of the flow is determined3:
The degree of manifestation of general symptoms - weakness, fever, the presence of enlarged lymph nodes. Changes in condition are also reflected in blood tests. With a mild form, the temperature rises to 37.5°C, with a moderate form up to 38°C, with a severe form - up to 40°C.
Syphilis
Syphilis is an infectious pathology caused by Treponema pallidum. Mouth ulcers are a typical symptom of syphilis that appears throughout the entire period of the disease. Moreover, the ulcers themselves undergo a certain development process:
- The ulcers are round in shape and have dense edges. They are painless and have a white coating.
- Over time, the ulcers begin to bleed slightly.
- After about 1-3 months, the ulcers heal, and in their place strong scars form, around which dense bluish edges are concentrated.
After defeating syphilis, dense scars still remain in the oral cavity. They are the most eloquent sign of a recent illness.
Treatment of syphilis is carried out in a closed venereology clinic. During remission, the oral cavity is treated with anti-inflammatory and antibacterial drugs.
Causes of ulcerative-necrotizing gingivitis
Ulcerative-necrotizing gingivitis is caused by fusobacteria and spirochetes. Most often it develops as a complication of catarrhal gingivitis, but it can also be an independent disease. It develops with poor oral hygiene against the background of a sharp decrease in immunity.
General factors
Common factors leading to the onset of the disease are stress, severe fatigue, infectious diseases, and hypothermia. More often the disease is observed in people with diseases of the digestive, endocrine and respiratory systems, heart and vascular diseases. Inadequate and unhealthy diet also increases the risk of developing ulcerative gingivitis. Taking certain medications can also lead to this disease.
Local factors
- Poor oral hygiene In this case, plaque accumulates on the teeth and stones form. With ulcerative necrotic gingivitis, not only ordinary microorganisms accumulate, but also spirochetes.
- Presence of other oral diseases Ulcerative gingivitis can occur as a complication of catarrhal gingivitis and herpetic stomatitis.
- Permanent gum injury For example, old fillings, crowns, dentures.
- Wisdom teeth eruption
- Multiple caries, as it increases the number of pathogens in the mouth
- Injury to the gums by the sharp edges of a carious cavity
- Oral surgery, including complex tooth extraction4
Gingivostomatitis in children
Most often in childhood, gingivostomatitis occurs, caused by the herpes virus.
The disease occurs in an acute form, usually of moderate or severe severity. Gingivostomatitis in a child begins with a sharp rise in temperature, lethargy, and headache. All these symptoms in children appear even before ulcers appear in the mouth, and they can easily be confused with signs of a cold or flu: there is a cough, runny nose, and sometimes diarrhea.
Upon examination, enlarged lymph nodes under the jaw and on the neck and reddened gums are detected. For 2-3 days, the oral mucosa becomes covered with ulcers, which are very painful. The illness lasts one to two weeks.
Treatment of gingivostomatitis consists of aseptic treatment and anesthesia of the oral cavity, as well as antiviral therapy and strengthening the immune system.
Symptoms of necrotizing ulcerative gingivitis
The disease develops quickly and rapidly, its symptoms appear very clearly.5,6
- Severe pain that gets worse with the slightest touch or temperature changes
- Swelling of the gums
- Sensitivity of the mucous membrane
- Spontaneous bleeding gums
- The tongue is covered with a green, yellow coating
- Ulcers appear on the surface of the gums, covered with a gray coating.
- A sharply unpleasant, strong odor from the mouth that does not go away even when brushing your teeth
- Increased temperature, weakness, fever
- Necrosis of gum tissue
- Brushing teeth and eating food is difficult
- Lymph nodes are enlarged
- Aches, muscle pain
This review examines acute herpetic stomatitis in children as the most common disease of viral etiology. Acute herpetic stomatitis (AHS), along with other inflammatory diseases of the oral mucosa in children, is usually accompanied by a decrease in general immunity. The authors recommend an integrated approach, including general and local treatment, with the use of immunomodulators, which will reduce the treatment time for acute herpetic stomatitis, reduce the severity of this disease and restore normal immunity in a shorter time.
Acute herpetic gingivostomatitis in children
Here is reviewed an acute herpetic gingivostomatitis in children as the most common disease of viral etiology. Acute herpetic gingivostomatitis (AHG) along with other inflammatory diseases of children's oral mucosa is generally accompanied by decrease in systematic immunity. The authors suggest the complex approach including general and local treatment with the application of immunomodulators that will reduce the terms of acute herpetic gingivostomatitis treatment, decrease the severity of this disease and in shorter terms recover normal immunity.
Acute herpetic stomatitis in children —
an infectious viral disease caused by primary contact with the herpes simplex virus, characterized by inflammation of the oral mucosa with the appearance of blistering rashes, increased body temperature and decreased immunity [1].
A third of the world's population is affected by herpes infection; over half of these patients suffer several attacks of infection per year, often including manifestations in the oral cavity. It has been established that the infection rate of children with the herpes simplex virus between the ages of 6 months and 5 years is 60%, and by the age of 15 it is already 90%. A similar situation is typical for dentistry, since the incidence of acute (primary) herpetic stomatitis in children increases every year.
The role of the herpes simplex virus in diseases of the oral mucosa was first pointed out at the beginning of the 20th century. N.F. Filatov (1902). He suggested the possible herpetic nature of the most common acute aphthous stomatitis among children. This evidence was obtained later, when antigens of the herpes simplex virus were discovered in the epithelial cells of the affected areas of the oral mucosa.
Acute herpetic stomatitis not only ranks first among all lesions of the oral mucosa, but is also included in the leading group among all infectious pathologies of childhood. Moreover, in every 7–10th child, acute herpetic stomatitis very early turns into a chronic form with periodic relapses [1].
Herpes simplex virus is a DNA virus. The size of the vibrio is 100-160 nm. Develops intracellularly. The virus is thermolabile and is inactivated at a temperature of 50-52°C for 30 minutes. At a temperature of 37°C, inactivation of the virus occurs within 10 hours. The virus persists for a long time at low temperatures (-70°C). It causes various diseases of the central and peripheral nervous systems, liver, other parenchymal organs, eyes, skin, gastrointestinal mucosa, genital organs, and also has a certain significance in the intrauterine pathology of the fetus. A combination of various clinical forms of herpetic infection is often observed.
Acute herpetic stomatitis has a relatively high contagiousness among non-immune individuals. The spread of the disease at the age of 6 months to 3 years is explained by the fact that at this age the antibodies received from the mother interplacentally disappear in children, as well as the lack of mature specific immune systems. Among older children, the incidence is significantly lower due to acquired immunity after a herpes infection in its various clinical manifestations.
Herpes infection, which manifests itself mainly in the oral cavity, is caused by the herpes simplex virus serotype 1 - HSV-1 (Herpes simplex virus HSV-1) [3]. Infection occurs through airborne droplets, contact and household routes (through toys, dishes and other household items), as well as from persons suffering from recurrent herpes of the lips.
In the development of herpetic infection, the structure of the oral mucosa in children in early childhood and the activity of local tissue immunity are of great importance. The highest prevalence of acute herpetic stomatitis in the period up to 3 years may be due to age-morphological indicators, indicating high permeability of histohematic barriers during this period and a decrease in morphological immune responses: thin epithelial cover with low levels of glycogen and ribonucleic acids, friability and low differentiation of the basement membrane and fibrous structures of connective tissue (abundant vascularization, high levels of mast cells with their low functional activity, etc.).
The pathogenesis of acute herpetic stomatitis has not been fully studied at present. In all cases, a viral infection begins with a violation of the integrity of the mucous membranes and skin, adsorption of viral particles and penetration of the virus into the cell. Further ways of spreading the introduced virus throughout the body are complex and poorly understood. There are a number of provisions indicating the spread of the virus by hematogenous and neural routes. During the acute period of stomatitis, viremia is observed in children.
The lymph nodes and elements of the reticuloendothelial system are of great importance in the pathogenesis of the disease, which is quite consistent with the pathogenesis of the sequential development of clinical signs of stomatitis. The appearance of lesions on the oral mucosa is preceded by lymphadenitis of varying severity. In moderate and severe clinical forms, bilateral inflammation of the submandibular lymph nodes often develops. All groups of cervical lymph nodes (anterior, middle, posterior) can be involved in the process. Lymphadenitis in acute herpetic stomatitis precedes rashes in the oral cavity, accompanies the entire course of the disease and remains for 7-10 days after complete epithelization of the rash elements.
Immune defense plays a certain role in the body’s resistance to disease and in its protective reactions. Both specific and nonspecific immune factors play a role in immune reactivity. Studies of nonspecific immune reactivity have established a violation of the body's protective barriers, which reflected the severity of the disease and the periods of its development. Moderate and severe forms of stomatitis sharply suppress natural immunity, which is restored 7-14 days after the child’s clinical recovery [1].
Primary infection usually occurs after 6 months of life, since before this the blood of most newborns contains antibodies to the herpes simplex virus, received from the mother transplacentally. Most often, the disease occurs between the ages of 1 and 5 years - 62-65% of cases. Children 4-5 years old account for 13-25%, then the incidence sharply decreases, amounting to 1-2 cases per 1000 in schoolchildren. The high incidence in children from 6 months to 3 years is explained by the fact that at this age antibodies received from the mother disappear , but there are still no mature systems of specific immunity and the role of nonspecific immunity is still small. Among older children, the incidence is much lower, since immunity is acquired after suffering a herpetic infection in one clinical form or another.
For the development of herpes infection, which primarily affects the oral cavity, the structure of the oral mucosa is of great importance. Thus, the highest prevalence of OGS in the period up to 3 years may be due to the high permeability of histological barriers during this period and a decrease in morphological immune responses, thin epithelial cover with low levels of glycogen and ribonucleic acids, friability and low differentiation of the basement membrane and fibrous structures of connective tissue.
Herpetic stomatitis can occur in newborn premature babies. It is believed that it is a consequence of ante- and perinatal infection, which is observed in 1/3 of cases.
Acute herpetic stomatitis, like many other childhood infectious diseases, occurs in mild, moderate and severe forms. The incubation period lasts from 2 to 17 days, and in newborns it can last up to 30 days. During the course of the disease, five periods are distinguished: incubation, prodromal, disease development, extinction and clinical recovery. During the development of the disease, two phases can be distinguished - catarrhal and rash of lesions.
Symptoms of damage to the oral mucosa appear in the third period of disease development. Intense hyperemia of the entire oral mucosa is observed; after a day, or less often two, lesions are usually found in the oral cavity. The severity of acute herpetic stomatitis is assessed by the severity and nature of the symptom of toxicosis and the symptom of damage to the oral mucosa.
The mild form of acute herpetic stomatitis is characterized by the external absence of symptoms of intoxication of the body; the prodromal period is clinically absent. The disease begins suddenly with an increase in body temperature to 37-37.5°C. The general condition of the child is quite satisfactory. Minor phenomena of inflammation of the nasal mucosa and upper respiratory tract may be detected. Sometimes hyperemia and slight swelling occur in the oral cavity, mainly in the area of the gingival margin (catarrhal gingivitis). The duration of the period is 1-2 days. The vesicle stage is usually not noticed by parents and doctors, since the vesicle quickly bursts and turns into erosion-aphtha. Afta-erosion is round or oval in shape with smooth edges and a smooth gray bottom with a rim of hyperemia around it.
In most cases, against the background of increased hyperemia, single or grouped lesions appear in the oral cavity, the number of which usually does not exceed five. The rashes are one-time only. The duration of the disease development is 1-2 days.
The period of extinction of the disease is longer. Within 1-2 days, the elements acquire a marble-like color, their edges and center are blurred. They are already less painful. After epithelization of the elements, the phenomena of catarrhal gingivitis persist for 2-3 days, especially in the area of the anterior teeth of the upper and lower jaws.
In children suffering from this form of the disease, as a rule, there are no changes in the blood, sometimes only towards the end of the disease a slight lymphocytosis appears. In this form of the disease, the protective mechanisms of saliva are well expressed: pH 7.4±0.04, which corresponds to the optimal state. During the height of the disease, an antiviral factor, interferon, appears in saliva (from 8 to 12 units/ml). The decrease in lysozyme in saliva is not pronounced.
Natural immunity in mild forms of stomatitis suffers slightly, and during the period of clinical recovery, the child’s body’s defenses are almost at the level of healthy children, i.e. in mild forms of acute herpetic stomatitis, clinical recovery means complete restoration of the body’s impaired defenses.
The moderate form of acute herpetic stomatitis is characterized by fairly clearly defined symptoms of toxicosis and damage to the oral mucosa during all periods of the disease. Already in the prodromal period, the child’s well-being worsens, weakness, moodiness, loss of appetite appear, catarrhal sore throat or symptoms of acute respiratory disease are observed. The submandibular lymph nodes enlarge and become painful. The temperature rises to 37-37.5°C.
As the disease progresses during the development of the disease (catarrhal phase), the temperature rises to 38-39°C, headache, nausea, and pale skin appear. At the peak of the rise in temperature, increased hyperemia and severe swelling of the mucous membrane, elements of a rash appear, both in the oral cavity and often on the skin of the face in the mouth area. In the oral cavity, from 10 to 20-25 lesions are usually noted. During this period, salivation increases, saliva becomes viscous and viscous. Marked inflammation and bleeding of the gums are noted.
Rashes often recur, as a result of which, when examining the oral cavity, one can see elements of the lesion that are at different stages of clinical and cytological development. After the first eruption of lesions, body temperature usually drops to 37-37.5°C. However, subsequent rashes are usually accompanied by a rise in temperature to the previous levels. The child does not eat, sleeps poorly, and symptoms of secondary toxicosis increase.
An increase in ESR up to 20 mm/h is noted in the blood, often leukopenia, sometimes slight leukocytosis; band leukocytes and monocytes are within the highest normal limits; lymphocytosis and plasmacytosis are observed. An increase in the titer of herpetic complement-fixing antibodies is detected more often than after a mild form of stomatitis.
The duration of the period of extinction of the disease depends on the resistance of the child’s body, the presence of carious and damaged teeth in the oral cavity, and irrational treatment. The latter factors contribute to the fusion of lesion elements, their subsequent ulceration, and the appearance of ulcerative gingivitis. Epithelization of the lesion elements takes up to 4-5 days. Gingivitis, severe bleeding of the gums and lymphadenitis last the longest.
With moderate disease, the pH of saliva becomes more acidic. The amount of interferon is less than in children with a mild form of the disease, but does not exceed 8 units/ml and is not found in all children. The content of lysozyme in saliva decreases more than in mild forms of stomatitis.
The severe form of acute herpetic stomatitis is much less common than the moderate and mild form. In the prodromal period, the child exhibits all the signs of an incipient acute infectious disease: apathy, adynamia, headache, skin-muscular hyperesthesia and arthralgia, etc. Symptoms of damage to the cardiovascular system are often observed: bradycardia and tachycardia, muffled heart sounds, arterial hypotension. Some children experience nosebleeds, nausea, vomiting, and pronounced lymphadenitis of not only the submandibular, but also the cervical lymph nodes.
During the development of the disease, the temperature rises to 39-40°C. The child develops a mournful expression on his face and is characterized by suffering, sunken eyes. A mild runny nose and cough are observed; the conjunctivae are somewhat swollen and hyperemic. Lips are dry, bright, parched. The mucous membrane of the oral cavity is swollen, clearly hyperemic, and acute catarrhal gingivitis is pronounced. After 1-2 days, elements of the rash begin to appear in the oral cavity (up to 20-25). Often, rashes in the form of typical herpetic blisters appear on the skin of the oral area, the skin of the eyelids and conjunctiva of the eyes, earlobes, on the fingers, like a panaritium. Rashes in the oral cavity recur and therefore, at the height of the disease in a seriously ill child, there are about 100 of them. The elements merge, forming large areas of necrosis of the mucous membrane. Not only the lips, cheeks, tongue, soft and hard palate are affected, but also the gingival margin. Catarrhal gingivitis turns into ulcerative-necrotic, with a sharp putrid odor from the mouth, profuse salivation mixed with blood. Inflammation on the mucous membrane of the nose, respiratory tract, and eyes worsens. Streaks of blood are also found in secretions from the nose and larynx, and sometimes nosebleeds are noted. In this condition, children need active treatment from a pediatrician and dentist, and therefore it is advisable to hospitalize the child in the isolation ward of a pediatric or infectious diseases hospital.
In the blood of children with a severe form of acute herpetic stomatitis, leukopenia, a band shift to the left, eosinophilia, single plasma cells, and young forms of neutrophils are detected. In the latter, toxic granularity is very rarely observed. Herpetic complement-fixing antibodies are, as a rule, always detected during the period of convalescence.
The reaction of saliva is acidic (pH 6.55±0.2), but after some time it changes to alkaline (8.1-8.4). Interferon is usually absent, the content of lysozyme is sharply reduced.
The period of extinction of the disease depends on timely and correctly prescribed treatment and on the child’s history of concomitant diseases.
Despite the clinical recovery of a patient with a severe form of acute herpetic stomatitis, profound changes in homeostasis are observed during the period of convalescence.
The diagnosis of acute herpetic stomatitis is established on the basis of anamnestic, epidemiological data, characteristic clinical symptoms, as well as cytomorphological data. Cytologically, the clinical diagnosis is confirmed by the presence in fingerprint smears, characteristic of herpetic infection, of epithelial cells with eosinophilic intranuclear inclusions, as well as giant multinucleated cells.
All children under observation undergo a complex of clinical, laboratory and instrumental studies, including a clinical blood test and immunological studies.
It is known that immunosuppression is one of the main factors in the implementation of herpes virus infection. In this regard, the state of local immunity of the oral mucosa is studied: the content of lysozyme, the level of immunoglobulins (in particular secretory IgA) in mixed saliva. The material for the study is smear impressions from the oral mucosa. Tests in which cell nuclei are stained with fluorescein and polymorphonuclear neutrophils and macrophages that are specifically stained with herpetic antiserum are observed as positive for herpes antigen; also determine the presence of virus-specific nucleotide sequences of the herpes simplex virus in swabs from the oral mucosa. For this purpose, the PCR method is used.
The essence of PCR diagnostics is to identify the pathogen using the indication of specific regions of the genome. The method provides high sensitivity and specificity for determining the infectious agent, starting from the earliest stages of the development of the infectious process. The material for research is scrapings from the oral mucosa.
Strepto-staphylococcal lesions (pyoderma)
The leading symptoms of the disease are caused by the addition of pyogenic microflora. Body temperature is elevated - in severe cases up to 38-39 ° C, signs of intoxication and lymphadenitis of regional nodes, prone to abscess formation, are expressed. On the red border and skin of the lips there are single or multiple purulent pustules, thick straw-yellow crusts; the surrounding skin is often hyperemic and infiltrated. The anterior parts of the oral mucosa may also be affected: lips, gums, tip of the tongue. In this case, against a hyperemic background, separate and merging erosions, covered with a loose coating, are revealed.
Vincent's ulcerative gingivostomatitis
Rarely observed in young children. In recent years, schoolchildren and teenagers also rarely get sick. The causative agents are considered to be saprophytes of the oral cavity: fusiform bacillus and spirochetes, which under certain conditions become pathogenic; they are found in large quantities in the discharge from the surface of ulcers.
The general condition of the child is serious, since the absorption of tissue decay products causes significant intoxication of the body, the body temperature is elevated, the regional lymph nodes are enlarged and painful, and salivation is increased. The gums are swollen, dark red in color; in the area of ulceration, the interdental papillae seem to be cut off due to the disintegration of the tissue at their apex and are covered with a dirty, soiled coating with a putrefactive odor [5].
The goals of treatment of acute herpetic stomatitis are:
— elimination of the cause of the disease;
- prevention of complications (streptostaphylococcal pyoderma, ulcerative necrotizing gingivostomatitis).
The doctor’s tactics when treating patients with acute herpetic stomatitis should be determined by the severity of the disease and the period of its development.
Indications for hospitalization:
- prolonged dehydration and intoxication;
- severe and complicated course of the disease.
Complex therapy for acute herpetic stomatitis includes general and local treatment. For moderate and severe disease, it is advisable to carry out general treatment together with a pediatrician. Due to the peculiarities of the clinical course of acute herpetic stomatitis, rational nutrition and proper organization of feeding the patient occupy an important place in the complex of therapeutic measures. Food must be complete, i.e. contain all the necessary nutrients and vitamins. Considering that the pain factor often forces the child to refuse food, first of all, before feeding, it is necessary to treat the oral mucosa with Cholisal gel, which provides a quick analgesic effect, topical anesthetics, a 5-10% oil solution of benzocaine or a gel containing lidocaine + chlorhexidine (lidochlor).
The child is fed predominantly liquid or semi-liquid food that does not irritate the inflamed mucous membrane. Much attention is paid to administering a sufficient amount of fluid. This is especially important during intoxication.
Local treatment for acute herpetic stomatitis requires the following tasks:
- relieve or reduce painful symptoms in the oral cavity;
- prevent repeated eruptions of lesions (reinfection);
- promote the acceleration of epithelization of lesion elements.
From the first days of the development of acute herpetic stomatitis, taking into account the etiology of the disease, serious attention should be paid to antiviral treatment. For this purpose, it is recommended to use ointment with bromonaphthoquinone (bonaftone ointment), tebrofen ointment, acyclovir ointment, interferon alpha-2 (viferon), herpferon, alpizarin ointment (0.5-2%), solution of leukocyte human interferon and other antiviral agents [1 ].
These medications are recommended to be used repeatedly (5-6 times a day) not only when visiting a dentist, but also at home. It should be borne in mind that it is advisable to use antiviral agents on both the affected areas of the mucous membrane and areas without rash elements, since they have a greater preventive effect than a therapeutic one. During the period of extinction of the disease, antiviral drugs and their inducers are replaced with anti-inflammatory and keratoplasty drugs.
Weak antiseptics and keratoplastics are of leading importance during this period of the disease. This is an oil solution of vitamin A, sea buckthorn oil, Vitaon oil, rosehip seed oil, ointments with methyluracil, solcoseryl, Actovegin (gel, ointment, cream, dental adhesive paste). The preparations are applied to the treated wound surface until complete epithelization.
The study of the state of local immunity in children with acute herpetic stomatitis made it possible to clarify the characteristic dynamics of various factors of local immunity in this disease. Thus, the content of IgA, which plays a major role in protecting the oral mucosa, correlates with the severity and nature of the pathological process. The content of lysozyme in saliva in patients with acute herpetic stomatitis depends on the severity of stomatitis and gingivitis. The revealed patterns of dynamics of indicators of local immunity of the oral cavity allow us to consider it pathogenetically justified to include drugs aimed at their correction in the complex treatment regimen for acute herpetic stomatitis. These drugs include immunomodulatory agents: imudon, glucosaminyl muramyl dipeptide (lycopid), azoximer bromide (polyoxidonium), lysobact, etc.
In case of severe damage, the elements of the skin rash are lubricated with salicylic-zinc paste (lassara) to form a thin crust in order to prevent complications (streptostaphylococcal pyoderma). Physiotherapeutic procedures are also used - ultraviolet irradiation and helium-neon laser irradiation.
It should be noted that acute herpetic stomatitis occurring in any form is an acute infectious disease, in all cases requiring the attention of a pediatrician and dentist in order to provide comprehensive treatment, eliminate contact of a sick child with healthy children, and carry out preventive measures for this disease in children's groups.
Treatment algorithm for children with acute herpetic stomatitis
Local treatment:
In the prodromal period, use 2-3 drops in the nose and under the tongue every 4 hours:
- human leukocyte interferon;
- meglumine acridone acetate (cycloferon).
The following are used as painkillers (before eating and before treating the oral mucosa):
- 5-10% suspension of benzocaine (anesthetic) in peach oil;
- lidocaine + chlorhexidine (lidochlor gel), Kamistad gel, 2% xylocaine solution [3].
To remove necrotic tissue and clean the mucous membrane and gingival margin and teeth from plaque, enzyme solutions are used: trypsin, chymotrypsin, chymopsin, ribonuclease, lysoamidase, etc.
For the purpose of antiseptic treatment of the oral cavity, the following groups of drugs are recommended:
- group of oxidizing agents (potassium permanganate, 1% hydrogen peroxide);
- cationic detergents (hexetidine solution (hexoral) or 0.02% chlorhexidine solution, miramistin solution);
- drugs of the nitrofuran series (furacilin); 1:5000 or 1:10000;
- corsodil solution or 0.02% chlorhexidine solution.
During the period of rashes, antiviral gels, ointments and solutions are recommended 3-4 times a day:
0.25% oxolinic, 0.25-1% tebrophenic, 2% alpizarin, 0.25-0.5% florenal, 1% bonafthonic, 0.25% adimalic, 5% liniment helepin or alpizarin, Viferon, solutions of interferon and reaferon [4].
During the period of extinction of the disease, anti-inflammatory and keratoplasty drugs are prescribed: solcoseryl jelly, Actovegin, Cholisal gel, Vitaon oil, Aekol, sea buckthorn oil, rosehip oil, etc. [4].
General treatment
V.M. Elizarova recommends the following general treatment regimen [5]:
Prescribe the following drugs as antipyretics and painkillers: paracetamol (tablets, syrup), efferalgan (tablets, syrup), panadol (syrup), calpol (syrup), cefekon in the form of suppositories (5-10 mg/kg body weight 3- 4 times a day), Tylenol (syrup, tablets), Nurofen (syrup), etc. Antihistamines are recommended - mebhydrolin (Diazolin), hifenadine (Fenkarol), loratadine (Claritin), clemastine (Tavegil), suprastin [1].
Among the antiviral drugs prescribed are acyclovir (5 mg per day can be used from 3 months of life), bonafton (0.025 g 1 to 4 times depending on age), alpizarin, meglumine acridone acetate (cycloferon), interferon alpha-2 (viferon -1 rectal suppositories).
Immunomodulatory drugs used in this treatment regimen are imunal, lycopid, polyoxidonium, lysobact, and immunomishki. In addition, drinking plenty of fluids and eating non-irritating foods is recommended.
Treatment of complications of acute herpetic stomatitis
Treatment of pyoderma includes removal of purulent crusts and treatment of the mucous membrane. The crusts are removed after application of anesthesia, having previously softened them with a 1% solution of hydrogen peroxide. The oral mucosa and erosive surfaces are thoroughly washed with antiseptic agents, treated with proteolytic enzymes, and then lubricated with antibacterial agents, for example, 2% lincomycin, 2% neomycin, erythromycin (10,000 units per 1 g), 10% dermatol and other ointments. If there is a history of allergic reactions to antibiotics, creams with glucocorticoids (fluorocort, flucinar, lorinden hyoxysone, etc.) are added to antibacterial ointments [5].
Treatment of Vincent's ulcerative gingivostomatitis is symptomatic.
Caring for a child with acute herpetic stomatitis
A sick child must be isolated from other children and report the disease to a child care facility if the child attends one.
In order to stop the spread of infection in children's institutions, it is necessary to disinfect premises, household items, toys with a 3% solution of chloramine B*, as well as quartzize the premises.
All children who have been in contact with sick people are lubricated with 0.25% oxolinic ointment on the mucous membranes of the nose and mouth or instilled in the nose with a solution of human leukocyte interferon, and also given ascorbic acid orally for 5 days.
The patient is given separate dishes, bed, and towel. He needs to stay in bed and follow all doctor's orders. Receive special food. Fresh vegetable decoctions in meat or fish broth are recommended, to which crushed boiled meat or fish or chicken fillet, and boiled vegetables are added. Warm low-fat milk and fermented milk products, soft-boiled eggs are beneficial. The patient's food can include freshly prepared, non-irritating juices from vegetables and fruits (for example, a mixture of carrot, cabbage and apple juices). Plenty of fluids and chemically and mechanically gentle food are recommended. Before eating, the oral mucosa should be numbed. To do this, first carefully lubricate the lips, and then the affected areas of the oral mucosa with an anesthetic emulsion. The emulsion is applied to the lips with the index finger wrapped in cotton wool. After eating, the oral cavity must be freed from food debris by rinsing the mouth with warm boiled water. For small children, the head is slightly lowered and the mouth is washed out with a rubber spray [5].
K.V. Tidgen, R.Z. Urazova, R.M. Safina
Kazan State Medical University
Dental clinic No. 9, Kazan
Tidgen Kristina Vladimirovna – graduate student of the Department of Pediatric Dentistry
Literature:
1. Pediatric therapeutic dentistry. National leadership / ed. VC. Leontyeva, L.P. Kiselnikova. - M.: GEOTAR-Media, 2010. - 896 p. (National Guidelines Series).
2. Persin L.S. Pediatric dentistry. — Ed. 5th, revised and additional / L.S. Persin, V.M. Elizarova, S.V. Dyakova. - M.: Medicine, 2003. - 640 pp.: ill. (Educational literature for students of medical universities).
3. Handbook of pediatric dentistry / ed. A. Cameron, R. Widmer; lane from English / ed. T.F. Vinogradova, N.V. Ginali, O.Z. Topolnitsky. — 2nd ed., rev. and processed - M.: MEDpres-inform, 2010. - 392 p.: ill.
4. Vinogradova T.F. Periodontal diseases and oral mucosa in children / T.F. Vinogradova, O.P. Maksimova, E.M. Melnichenko. - M.: Medicine, 1983. - 208 p.: ill.
5. Selected reports and lectures on dentistry / Intro. Art. acad. RAMS E.I. Sokolova. - M.: MEDpress, 2000. - 140 p.
Diagnosis of necrotizing ulcerative gingivitis
Diagnosis is made through the clinical manifestations of necrotizing ulcerative gingivitis.7,8
During the examination and questioning, the dentist identifies poor hygiene, bleeding gums, poor general condition and the absence of gum pockets (impaired attachment of the gum to the tooth). Be sure to take a panoramic photograph of all teeth to distinguish ulcerative gingivitis from periodontitis.
Additionally, bacteriological examination and the ELISA method can be carried out to confirm the diagnosis, determine the level of immunoglobulins and select appropriate treatment tactics.
It is important to distinguish ulcerative gingivitis from immunodeficiency conditions and blood diseases. For this purpose, if necessary, other tests may be prescribed.
Gingivitis: treatment at home
Once again, let us draw your attention to a very important point - treatment of gingivitis in adults at home is only possible in terms of a course of anti-inflammatory therapy. At home, you can successfully use antiseptic rinses and applications to treat catarrhal gingivitis, but to remove plaque, you still need to visit the dentist!
A small example: a person’s gums are bleeding and he decides to use the remedies he heard about in an advertisement. These can be various gels, rinses or anti-inflammatory toothpastes. And indeed, as long as a person uses such means, bleeding decreases or disappears completely for a while. But as soon as the use of the products is stopped, the gums begin to bleed again, plus their swelling and redness return.
The reason for this is quite commonplace - the person tried to treat the symptoms (such as bleeding, pain, swelling) without removing the cause of these symptoms (microbial plaque, as well as hard supra- and subgingival dental plaque). Advertisements for various dental products do not talk about the causes of bleeding or the need to remove dental plaque. Moreover, for obvious reasons... We hope that our article on the topic: Gingivitis symptoms and treatment in adults was useful to you!
Sources:
1. Dental education of the author of the article, 2. Based on personal experience as a periodontist, 3. National Library of Medicine (USA), 4. American Academy of Periodontology (USA), 5. “Non-surgical periodontal treatment” (Roncati M.).
Treatment of ulcerative-necrotizing gingivitis
At the first signs of illness, consult a doctor immediately!
Treatment of ulcerative gingivitis is always complex:
- Anesthesia of the oral cavity with sprays, gels, solutions. With ulcerative gingivitis, this stage is extremely important, since the pain is quite severe.
- Removing the inflammatory process. To do this, use gentle methods to remove plaque and tartar, and be sure to prescribe a course of rinsing with antiseptics for up to two weeks. It is during this visit to the doctor that material is taken for bacteriological examination.
- Removal of general symptoms - fever, headache, for this purpose analgesics and antipyretics are prescribed.
- Destroying pathogenic bacteria, for this purpose antibacterial or antimicrobial drugs are prescribed. (Important! Prescribed strictly by your doctor!)
- Vitamin therapy – to increase the body’s overall resistance to harmful factors.
- During treatment, it is recommended to eat non-irritating foods with sufficient calorie content and not to use spices.
- Treatment of general diseases together with a therapist, gastroenterologist and other specialists.
- After acute inflammation subsides, epithelializing drugs are prescribed (to stimulate tissue healing), professional hygiene, treatment of caries and its complications, removal of wisdom teeth, fillings and crowns (if necessary).
In case of ulcerative gingivitis, it is necessary to strictly follow all the doctor’s recommendations, otherwise complications may arise, and the disease may become chronic.
Removal of dental plaque is carried out under local anesthesia of the gums, using antiseptic drugs, only with the help of hand instruments.
Medicinal preparations containing metronidazole and chlorhexidine are applied to the ulcers, cleared of plaque with special enzymes. These drugs are designed to destroy pathogenic microorganisms, but they should be used only as prescribed by a doctor to avoid complications.
To relieve the inflammatory reaction, local applications with an NSAID solution can be applied for 10-15 minutes.
Recurrent necrotizing peryadenitis
Recurrent necrotizing peryadenitis is also called Setton's aphthae. Its symptoms are:
- Seals appear in the submucosa of the oral cavity;
- Instead of compactions, ulcers with raised edges develop over time;
- The ulcers become inflamed, causing blood and lymphatic discharge.
Places where such afts accumulate are the upper and lower lips, cheeks and sides of the tongue. The pathology is characterized by extremely severe pain. Patients find it so difficult to eat that many give up eating completely. Difficulties also arise during conversation. The healing process of aphthae lasts a long time - sometimes up to several months, and the pathology itself persists for up to several years.
Treatment of necrotizing ulcerative gingivitis with Tantum® Verde
Effective treatment of ulcerative gingivitis is possible with the use of anti-inflammatory drugs, which include Tantum® Verde . Benzidamine in its composition has a complex effect on the gums: reduces swelling, relieves inflammation, reduces pain and kills microbes on the surface and inside the affected tissues. Benzidamine penetrates well into the mucous membranes, which allows you to quickly cope with the disease. Tantum®Verde allows you to quickly relieve pain9, which is especially important in the treatment of necrotizing ulcerative gingivitis. From the first minute, Tantum® Verde has an anti-inflammatory and local anesthetic effect on the symptoms of gingivitis, such as a burning sensation, swelling and swelling of the gums. After the acute effects have subsided, it is possible to dissolve Tantum® Verde , since they have an anti-inflammatory effect within 9 minutes, which will allow you to quickly cure gingivitis.10, 11, 12
Traumatic mouth ulcers
The name of traumatic ulcers speaks for itself. This is the appearance of wounds in the oral cavity due to injury to the mucous membrane. The causes of injury may be:
- Bite of the mucous membrane;
- Accidental contact with a toothbrush;
- Inaccurate dental treatment.
One of the types of traumatic ulcers are prosthetic ulcers - wounds formed due to incorrect sizes of removable dentures. They are localized precisely under the dentures.
Healing of traumatic ulcers lasts 1-2 weeks. As a rule, this is a one-time pathology that goes away on its own without additional treatment. Such aphthae are painless and small in size.
If a complication of the disease nevertheless begins, it is necessary to visit a doctor so that he can prescribe anti-inflammatory and antibacterial medications to completely eliminate the pathology.
Prediction and prevention of necrotizing ulcerative gingivitis
If you consult a doctor in time and receive quality treatment, a full recovery is possible. Recurrence of the disease occurs with exacerbation of chronic diseases, a sharp decrease in immunity and poor oral hygiene.
If you postpone going to the doctor and do not follow the recommendations, ulcerative gingivitis can become chronic, which is less treatable, or develop into a more serious disease - periodontitis, which is accompanied by loss of bone tissue. Therefore, it is important to take a responsible approach to the treatment of this disease.
If a person has suffered ulcerative gingivitis, then a second visit is scheduled after 1-2 months, and then you should visit the dentist every six months.
Prevention of ulcerative gingivitis:
- Regular and adequate teeth cleaning
- Visit your dentist for examination and treatment (if necessary) twice a year
- Strengthening the immune system: you should pay attention to such simple things as physical exercise, proper nutrition, sleep patterns, hardening
- Stress management
- Treatment of existing chronic diseases: it is important to avoid exacerbations, otherwise relapses of the disease are inevitable
- Taking vitamins
Diagnosis and treatment of the disease
The diagnosis is established on the basis of laboratory diagnostics. Numerous lesions of an ulcerative or necrotic nature are found on the mucous membrane of the oral cavity. The final diagnosis is made based on a blood test and bacterioscopic examination.
Treatment of the disease consists largely of the use of various methods of local therapy. Pain is relieved with anesthetics. An important role is played by the use of gels and ointments with antibacterial properties.
The sores need to be thoroughly cleaned, and this is best done surgically. This technique may include keratoplasty followed by sanitation of the oral cavity.
The course of treatment also includes the use of antibiotics and anti-inflammatory drugs. With timely detection and treatment of pathology, the prognosis is favorable.