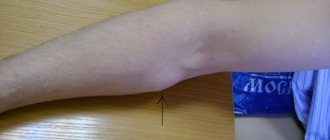
Types of postoperative scars
Keloid.
A lumpy scar made of overgrown connective tissue that is red or bluish in color. It looks like a tumor or a mushroom cap. The size of the keloid scar is larger than the wound itself, it hurts, itches, and sometimes pulsates.
Hypertrophic.
Outwardly similar to a keloid, but its size does not extend beyond the wound. A hypertrophic scar does not cause any discomfort and lightens over time.
Normotrophic.
A well-healing scar is initially convex and reddened, after 3 months it becomes almost invisible, there is no sensitivity.
Recommendations for the rehabilitation period
In order for the body to recover successfully and in a short time, the patient should adhere to a number of medical recommendations in the so-called late postoperative period.
- Wearing a bandage
. A support corset is especially recommended for women with weak abdominal muscles and a history of multiple births. - Sex life
. To avoid infection and injury, sex should be postponed for 1 -1.5 months until the wounds are completely healed. - Carrying weights
. In order to prevent abdominal bleeding and suture dehiscence, heavy lifting and physical activity should be limited for the same period. - Intimate gymnastics
. To prevent prolapse of the uterine stump, prolapse of the vaginal walls and urinary incontinence, Kegel exercises are performed using a simulator to improve the muscle tone of the vagina. - Diet
. In order to avoid disruption of the gastrointestinal tract, it is necessary to review your usual diet and exclude fatty, fried and smoked foods from it. Preference should be given to foods high in fiber, vegetables and fruits.
Hysterectomy certainly affects a woman’s psycho-emotional state. She needs the support of her family and friends more than ever. This operation is a huge blow for patients who have indications for it, and it is even more saddening for young women whose uterus was removed as a result of medical error. The realization that they will never be able to get pregnant again leads them to depression.
I would like to note that an alternative to becoming a mother naturally does exist and this is surrogacy.
If you dream of experiencing the joys of motherhood, but due to the fault of a doctor you have lost your reproductive function - fill out an application on our website, and we will provide you with a surrogate mother ready to bear your child! Legal aspects related to proof of medical error are ready to be resolved by our specialists who have sufficient experience in this matter.
Complications of postoperative scars
Ligature fistula of a postoperative scar.
At the site of the suture, an inflamed hollow canal (hole) is formed, from which pus, sometimes urine and feces, are released. The cause of the complication is infection entering the body through the suture or an allergy to the threads with which the wound was sutured. The fistula can develop into an abscess, cellulitis or sepsis.
Infiltrate of postoperative scar.
This is a seal at the site of the suture, inside of which pus accumulates. The infiltrate is very painful to the touch, hot, red. Occurs due to infection of the suture.
Granuloma of a postoperative scar.
At the site of the scar, as a reaction to foreign bodies (suture threads), granulomas appear - nodules of dense tissue up to 2 mm in diameter, sometimes they contain pus. Granulomas are accompanied by an increase in the patient's body temperature.
Endometriosis of postoperative scars.
Occurs after gynecological operations on the uterine cavity, due to endometrial particles entering the wound. Patients feel pain in the scar area, blood is released from the suture, and dense nodules appear on the scar.
Treatment of complications of postoperative scars can be either surgical or conservative. Ligature fistula and infiltration usually require surgical intervention and re-suturing of the wound. Granulomas most often resolve on their own, but require aseptic treatment and medical supervision. When treating scar endometriosis, hormonal medications are prescribed.
Aesthetic surgery methods are used to remove keloid scars.
Treatment of long-term non-healing postoperative wounds of the perineum and anal canal
According to the definition of a special meeting of the European Society for Tissue Repair, “a wound should be considered chronic if it does not heal within a period that is normal for wounds of this type or location” [7]. According to our data, a wound process that exists for more than 45 days without signs of active healing is considered chronic.
Recently, the number of patients infected with sexually transmitted microorganisms continues to grow steadily. Sexually transmitted diseases (STDs) are often asymptomatic or minimally symptomatic, so many patients do not consult a doctor; in this regard, sexually transmitted infections have a strong tendency to become chronic [2].
In perineal wounds after surgical interventions, there are polymicrobial associations represented by opportunistic bacteria [3], including clinically significant ones, in combination with chlamydia, trichomonas, gardnerella, mycoplasma, ureaplasma, cytomegalovirus (CMV), genital herpes (virus herpes simplex type 2 (HSV-2)), as well as candida, i.e., sexually transmitted pathogens [1, 4, 8, 11, 12].
However, there are very few works devoted to this problem; they mainly concern gynecological and urological practice. In this regard, to study the influence of sexually transmitted infections on the course of the wound process, we decided to study the microbiocenosis of postoperative wounds in patients after operations on the distal rectum, anal canal and perineum.
A study was conducted, the purpose of which was to study wound microbiocenosis and develop a complex of specific corrective therapy in the postoperative period, aimed at improving the results of treatment of patients with long-term non-healing wounds of the anal canal and perineum.
Materials and methods
The study has been conducted from September 2010 to the present. The study included 96 people who underwent surgery at the State Scientific Center of Coloproctology for rectal fistulas, chronic anal fissures and hemorrhoids.
The main group consisted of 49 patients with a sluggish wound process, confirmed by clinical cytological examination, which resulted in long-term non-healing wounds (46 to 118 days passed from the day of surgery, on average 81.3 ± 49.3). The control group consisted of 47 patients, in whom, according to clinical and cytological studies, no deviations in the course of the wound process were noted; the wounds healed in normal periods - on average 37±10.5 days (p<0.05).
A comparative analysis of 2 groups of patients did not reveal significant differences in gender and age composition. Thus, in the main and control groups there were more men - 28 (57.1%) and 29 (61.7%), respectively. There were 21 (42.9%) women in the main group, and 18 (38.3%) in the control group.
The age of the patients in the main group ranged from 19 to 74 years, but most of them were people of working age, their average age was 41.0±13.2 years. In patients in the control group (persons from 18 to 72 years old), the average age was 42.8±12.2 years.
The patients were also comparable in terms of nosological forms. Among the 49 patients of the main group, there were 13 (26.5%) patients with chronic anal fissures, 28 (57.1%) with rectal fistulas and 8 (16.3%) with hemorrhoids. The majority of patients in the control group - 24 (51.1%) were also diagnosed with fistulas, 13 (27.7%) had fissures and 10 (21.3%) had hemorrhoids.
There were also no significant differences in the nature of surgical interventions. In most cases, patients in both the main and control groups underwent surgical interventions involving excision of fistulas into the lumen of the rectum: in 21 (42.9%) and 17 (36.2%), respectively. Excision of fistulas with sphincter suturing was performed in 3 (6.1%) patients in the main group and in 5 (10.6%) patients in the control group. Excision of the fistula with reduction of the flap was performed in 4 (8.2%) patients in the main group and 2 (4.3%) in the control group.
21 (42.8%) (11 men and 10 women) patients in the main group had indications of a history of STDs and diseases that could be caused by sexually transmitted infections, while patients in the control group had no indications of such diseases. in one observation (p<0.001). The following diseases were identified in the patients of the main group: 2 (4.1%) were observed by a urologist for chronic prostatitis; 2 (4.1%) patients were diagnosed with colpitis in the past, but the causative agents of this disease were not identified; indication of previous adnexitis occurred in 1 (2.0%) patient; 1 patient (2.0%) was treated for Reiter's syndrome; 5 men (10.2%) suffered from trichomoniasis; 3 patients (6.1%) (a woman and two men) – chlamydia; 2 patients (4.1%) had gardnerellosis and 3 (6.1%) had candidiasis, as well as 1 (2.0%) had genital herpes; 1 patient (2.0%) had ureaplasmosis in the past (Table 1).
In all patients in the postoperative period, bacteriological and bacterioscopic examinations of wound discharge from the anal canal and urethra were carried out; in women, additionally from the cervical canal: in patients of the control group - on the 25th day after surgery and in patients of the main group - at the time of treatment, and then 14 days after the start of treatment.
Using a light microscope, the causative agents of infections such as trichomoniasis, candidiasis, gardnerellosis, and the presence of gram-positive and gram-negative cocci and rods were determined. In addition, the polymerase chain reaction (PCR) method was used to diagnose sexually transmitted infections. In all patients in whom chlamydia, mycoplasma, ureaplasma, and gardnerella were detected, the diagnosis was confirmed by direct immunofluorescence. When HSV-2 and CMV were detected, the diagnosis was confirmed using the culture method. Microbiological studies were carried out in a bacteriological laboratory using a technique that allows us to determine the quantitative content and species spectrum of aerobic and facultative anaerobic microorganisms.
In patients of the main group, immediately after treatment for a long-term non-healing wound (on the 46th–118th day), and then 14 days after the start of treatment, cytological and pathomorphological studies of discharge from postoperative wounds were carried out. In patients in the control group, these studies were carried out on the 25th day after surgery.
results
During a cytological examination during treatment for a long-term non-healing wound, 45 (91.8%) patients of the main group showed a picture of “perverted” repair - the presence of multinucleated cells such as foreign bodies in smears from wounds, and also in all 49 patients - chronic inflammatory process with a large number of unchanged leukocytes. The number of leukocytes in wounds from 30 to 40 per field of view was observed in 8 (16.3%) patients, 40–60 in 7 (14.3%), 60–80 in 9 (18.4%), the entire field vision – in 25 (51%) patients. By the 25th day, in all patients in the control group, leukocytes with signs of dystrophy were in small numbers and did not exceed 5 per field of view (p <0.001).
The cytological examination data correlated with the data obtained during the pathomorphological examination. In patients of the main group, a large number of unchanged neutrophils were found in the biopsy specimen; the microflora is localized both extra- and intracellularly; the phenomena of phagocytosis are weakly expressed. In patients in the control group, the biopsy specimen revealed single, dystrophically altered leukocytes, as well as macrophages and fibroblasts.
During microbiological examination at the time of treatment (46–118 days after surgery), various microorganisms were identified in the discharge of postoperative wounds in all 49 (100%) patients of the main group; In patients in the control group, on the 25th day after surgery, in 44 (93.6%) of 47 observations, any microorganisms were detected, and in 3 (6.4%) of them there was no growth in bacterial cultures.
In patients of the main group, Enterococcus faecalis (fecal streptococci) predominated among microorganisms - in 28 (57.1%), as well as Escherichia coli (Escherichia coli) - in 20 (40.8%); the former occurred more than 4 times more often, the latter – 6 times more often than in patients in the control group. Enterobacter cloacae (Enterobacter) was found 11 times more often in patients of the main group compared to patients in the control group (this microorganism was found in only 1 patient in the control group). Candida albicans (yeast fungus) was cultured in 14 (28.6%) patients in the main group and in 9 (19.1%) in the control group.
In patients of the main group, in bacterial cultures from postoperative wounds such clinically significant microorganisms as Proteus mirabilis (Proteus) were found in 10 (20.4%), Acinetobacter lwoffii (Acinetobacter) - in 4 (8.2%), Staphylococcus aureus (Staphylococcus aureus) – in 10 (20.4%), Streptococcus haemolyticus (hemolytic streptococcus) – in 3 (6.1%) observations. The total frequency of detection of these clinically significant opportunistic microorganisms in patients of the main group was 27 (55.1%) cases, the number of microorganisms exceeded 105 CFU. In patients in the control group, clinically significant microorganisms were detected only in 1 (2.1%) patient (Staphylococcus aureus was cultured); the microbial number in this case was 105 CFU (p <0.001).
Associations of microorganisms in bacterial cultures were found in 47 (95.9%) patients of the main group: 5 different pathogens were found in 5 (10.2%), 4 in 5 (10.2%), 3 in 5 (10.2 %), 2 – in 32 (65.3%) patients; whereas in the control group, only 4 (8.5%) patients had an association of 2 microorganisms (p <0.001) (Table 2).
In all patients of the main group with long-term non-healing wounds, various sexually transmitted microorganisms were identified, of which pathogenic STD pathogens were found in 98% of patients, while in the control group this figure was only 23.4% (in 11 out of 47 patients), Moreover, all detected microorganisms that cause STDs in the latter were opportunistic (p <0.01) (Fig. 1).
In 26 (53.1%), i.e. more than half of the patients in the main group, chlamydia was detected in the wound discharge. At the same time, Chlamydia trachomatis was also found in the urethra and cervical canal of women in only 3 (6.1%) patients. In the control group, chlamydia was not diagnosed (p<0.001).
Trichomonas was detected in more than a third of patients of the main group - in 19 (38.8%) cases: in 2 (4.1%) patients in discharge from wounds, as well as the urethra, anal and cervical canals, and in 2 (4.1%) %) of men - in the urethra and discharge from wounds, and in 15 (30.6%) patients - only in discharge from postoperative wounds. Trichomoniasis was not detected in the control group (p<0.001).
Gardnerella was detected in 17 (34.7%) patients of the main group: in 8 (16.3%) of them this microorganism was found in all the studied material, in 9 (18.4%) - only in the wound discharge. In 7 (14.9%) patients in the control group, this microorganism was detected in 5 (10.6%) observations in the entire study material, in 2 (4.3%) - only in discharge from the urethra and cervical canal.
Candida was detected in 29 (59.2%) cases in patients of the main group in discharge from the anal canal, urethra, cervical canal and postoperative wounds. In the control group, candidiasis was found in 5 (10.6%) people also in the entire study material (p <0.001).
Somewhat less common were intracellular microorganisms such as ureaplasma and mycoplasma. In 6 (12.2%) patients of the main group, ureaplasma was detected in all the studied material, while in the control group this microorganism was detected in 1 (2.1%) patient only in the discharge from the urethra (p <0.05). In 1 (2.0%) case, a patient in the main group was diagnosed with Mycoplasma hominis, which was detected in the discharge of postoperative wounds and the anal canal. In 1 (2.1%) patient in the control group, Mycoplasma hominis was found in the discharge of the postoperative wound and urethra.
In 6 (12.2%) patients of the main group, HSV-2 was detected: in 3 (6.1%) in material from the urethra, cervical canal and postoperative wounds and in 3 (6.1%) only in discharge from wounds. HSV-2 was not found in the control group (p<0.05).
CMV was detected in 10 (20.4%) patients of the main group: in 9 (18.4%) in the anal canal and wound discharge and in 1 (2.0%) patient in the urethra, cervical canal and wound discharge; whereas in the control group it was not detected in any observation (p <0.001).
The frequency of detection of Trichomonas in patients of the main group only from discharge from postoperative wounds in the absence of them in discharge from the genitals was 30.6% (in 15 observations), chlamydia - 46.9% (in 23 observations), CMV - 18.4% ( in 9 observations) and HSV-2 – 6.1%. This fact indicates a long-term chronic process, in which it can be difficult to detect STD pathogens if there is no provoking factor. Since the causative agents of chronic sexually transmitted infections are in the epithelial cell in an inactive, “dormant” state, the appearance of a wound in the perineal area or anal canal is the very provoking factor that allows the chronic latent infection to become active.
STD pathogens in all 49 patients of the main group in whom they were diagnosed were not found as a monoinfection in any observation, but were found only in association with other STD pathogens. The presence of 2 microorganisms causing STDs was found in 33 (67.3%) patients, and in 16 (32.7%) patients of the main group a combination of 3 pathogens was found.
In 11 patients in the control group in whom sexually transmitted microorganisms were identified, on the contrary, 1 pathogen was most common - in 8 (17.0%), a combination of 2 microorganisms was detected in 3 (6.4%) patients, and the presence of 3 or more microorganisms at once was not detected in any observation (p <0.001).
In patients of the main group, the frequency of detection of associations of microorganisms was: Trichomonas, CMV and Candida - 10.2% (5 patients); chlamydia, trichomonas and candida – 8.2% (4 patients); trichomonas, gardnerella and candida – 10.2% (5 patients); chlamydia and gardnerella – 20.4% (10 observations); chlamydia and candida – 14.3% (7 patients); trichomonas and candida – 8.2% (4 cases). In 3 (6.4%) patients in the control group, Candida was found in combination with Gardnerella.
Among the associations of opportunistic microorganisms with STD pathogens in patients of the main group, there were combinations: Staphylococcus aureus with Trichomonas, chlamydia and candida - in 4 (8.2%) patients; Protea with Trichomonas and Candida – in 3 (6.1%); Proteus with chlamydia and candida – in 6 (12.2%). As already indicated, Staphylococcus aureus was detected in culture only in 1 (2.1%) patient in the control group and was associated with candida.
Hemolytic streptococci were associated with enterococci, chlamydia, candida and HSV-2 in 2 (4.1%) patients, in association with chlamydia and candida - in 1 (2.0%) patient of the main group.
Thus, opportunistic, clinically significant microorganisms are often associated with pathogenic microorganisms, which include Trichomonas, Chlamydia, CMV and HSV-2. It can be said that sexually transmitted pathogenic microorganisms create favorable conditions for the proliferation of opportunistic microorganisms, such as Staphylococcus aureus, Proteus, hemolytic streptococcus, etc., which in turn leads to long-term maintenance of the inflammatory wound reaction and slowdown of repair processes in wounds
All patients with long-term non-healing wounds in whom STDs were detected were prescribed appropriate therapy depending on the pathogen isolated.
For chlamydia, antibiotics were prescribed, taking into account that the anti-chlamydial agent should actively act on dividing reticular bodies. These antibiotics include: macrolides (roxithromycin, clarithromycin, josamycin), tetracyclines (tetracycline, doxycycline), erythromycin, fluoroquinolones (ciprofloxacin, ofloxacin).
For mycoplasmosis and ureaplasmosis, patients received antibiotics from the following groups: macrolides (roxithromycin, clatrithromycin, josamycin), tetracyclines (tetracycline, doxycycline), fluoroquinolones (ciprofloxacin, ofloxacin), lincosamines (lincomycin, clindamycin), aminoglycosides (gentamicin, streptomycin).
For trichomoniasis and gardnerellosis, drugs with antiprotozoal and antimicrobial effects were used: metronidazole, tinidazole, ornidazole.
Treatment of candidiasis was carried out with antimycotic drugs from the groups of triazole (fluconazole, itraconazole), imidazole, polyene (nystatin, levorin, amphotericin B), allylamine, echinocandin (caspofungin).
For genital herpes, interferon and compounds with interferon-inducing activity were prescribed; inhibitors of viral nucleic acid replication (nucleoside analogs (acyclovir), pyrophosphate analogs (foscarnet sodium)).
For CMV infection, inhibitors of viral nucleic acid replication were prescribed: ganciclovir, pyrophosphate analogues (foscarnet sodium), potato shoot extract.
All patients were prescribed probiotics in combination with etiotropic drugs to restore normal flora of the gastrointestinal tract.
As a result of the treatment, recovery was noted in all patients with long-term non-healing wounds included in the main group, which was confirmed by clinical, cytological and pathomorphological studies.
Clinical example: patient V., operated on for a transsphincteric fistula of the rectum. She applied for a long-term non-healing wound on the 56th day after surgery. In the wound area, hypergranulations were detected, which bled easily upon contact; in some areas the wound was covered with fibrin (Fig. 2).
PCR and bacterioscopic examination of discharge from the wound revealed trichomonas, chlamydia and candida. After 3 weeks After specific therapy aimed at eliminating identified infectious agents, the wound healed completely.
Clinical example: patient K., operated on for an extrasphincteric fistula of the rectum. On the 108th day after surgery, upon clinical examination, there was copious discharge from the wound of a mucopurulent and mucous-sacral nature (Fig. 3).
Clinical examination data correlated with cytological (Fig. 4) and pathomorphological (Fig. 5) studies. PCR and bacterioscopic examination of discharge from the wound revealed CMV, HSV-2 and candida. After etiotropic treatment (antiviral therapy, antimycotic drugs), the wound healed completely.
Conclusion
1. In patients with a history of long-term non-healing postoperative wounds, the frequency of detected genitourinary infections and diseases possibly caused by STDs was 42.8%, while in patients in the control group there were no anamnestic indications of previous STDs (p <0.001).
2. During cytological examination, smears from wounds showed a picture of perverted repair in 91.8% of patients in the main group. In all patients in the control group, by the 25th day, leukocytes were found only in small quantities (up to 5 per field of view), with signs of dystrophy (p <0.001).
3. The frequency of detection of such clinically significant microorganisms as Proteus, hemolytic streptococci, Staphylococcus aureus, Acinetobacter in patients of the main group was 55.1%. And only 1 (2.1%) patient in the control group was cultured with Staphylococcus aureus (p <0.001). Associations of microorganisms in bacterial cultures were found in 95.9% of patients in the main group, while in the control group - only in 8.5% of patients (p <0.001).
4. All patients of the main group with long-term non-healing wounds had various STDs, including obligate pathogenic microorganisms in 98%. In 23.4% of patients in the control group, the detected sexually transmitted microorganisms were only opportunistic (p <0.01).
5. In the majority of patients with long-term non-healing wounds, trichomonas (30.6%), chlamydia (46.9%) and CMV (18.4%), herpes viruses (6.1%) were detected only in the discharge from the wounds and were not detected in scrapings from the genitals. The presence of a wound defect in the perineal or anal canal is a provoking factor that allows a chronic, latent infection to become active.
6. Clinically significant opportunistic pathogens (Proteus, Acinetobacter, hemolytic streptococcus, and Staphylococcus aureus) are most often associated with sexually transmitted pathogens, which include Trichomonas, Chlamydia, CMV, and HSV-2.
How to prevent bleeding?
To avoid postoperative bleeding, you must refrain from the following actions:
- eat hard, rough, hot and cold foods;
- rinse your mouth intensively, especially with hot water;
- take a hot bath or visit a sauna;
- engage in heavy physical labor;
- actively use facial expressions (open your mouth wide, etc.);
- clean the affected area with a toothbrush, touch the wound with your tongue, fingers or foreign objects;
- smoke, drink alcohol;
- apply warm compresses to the cheek.
Normal socket healing
The above conditions must be observed for at least 24 hours (ideally 3 days) - this will help avoid not only bleeding, but also serious postoperative consequences.
In most cases, bleeding after tooth extraction is a normal physiological phenomenon that can be eliminated with simple home remedies, and if you follow all the doctor’s recommendations, the pain, fear and blood that accompany any operation will soon be left behind.
- What medicine is put into the hole after tooth extraction?
Causes of bleeding after tooth extraction
Bleeding after dental surgery is usually divided into primary and secondary - in the first case, blood flows immediately after the procedure, and secondary bleeding can develop several hours, sometimes several days after the visit to the clinic.
Bleeding after tooth extraction
There can be several reasons for primary bleeding, most of them are associated with pathological conditions of the body.
Table. Causes of primary bleeding after tooth extraction.
| Causes of bleeding | How to prevent |
| High blood pressure | Before going to the dentist, you need to measure your pressure and also take a sedative that will reduce the risk of it (pressure) increasing during the operation |
| Poor blood clotting in certain diseases (leukemia, hepatitis, hemophilia) | People with serious pathologies and hematopoietic diseases should report their problem to the doctor, who will choose the safest method of performing the operation |
| Taking medications | 2-3 days before tooth extraction, refrain from taking aspirin, heparin and other blood thinning drugs, as well as oral contraceptives (increased concentrations of estrogen in the blood in women can also cause bleeding) |
| Severe stress | If a person has a strong fear of dental procedures, a surge of adrenaline in the body can provoke bleeding - to prevent it, before visiting the dentist you need to try to calm down, and if necessary, take a sedative |
| Anatomical features of the dentofacial apparatus (large blood vessels on the surface of the gums) | Closely monitor the condition of the socket after surgery, avoid physical activity and follow the doctor’s recommendations |
- Why do my gums hurt after tooth extraction?
Another common cause of severe gum bleeding after tooth extraction is medical errors during extraction. Careless or too rough operation causes severe tissue trauma, which causes intense bleeding, and this situation is especially dangerous when large branches of the arteries are damaged.
Severe bleeding may be the result of a medical error
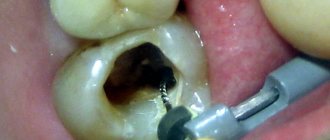
The main cause of secondary bleeding is patients’ failure to comply with the dentist’s recommendations: drinking hot drinks, solid foods, exposure to other traumatic factors, smoking, etc. In addition, blood from the socket can ooze in the event of complications developing - suppuration, alveolitis, the presence of cysts or granulomas. They impair coagulation at the site of inflammation, which leads to large blood loss both during and after surgery.
Alveolitis in the tooth socket